EHR Systems in Acute Care: The Cellma Advantage

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Your browser does not support the audio tag. Table of Contents In acute care, every second matters. Yet, healthcare teams working across hospitals still face fragmented data, paper-based documentation, and fragmented communication which all contribute to unnecessarily slow critical decision-making. Between 2022 and 2023, hospitals in England had 16.4 million finished admission episodes, 2.6% more than the previous year. In April 2025, A&E departments recorded 396,900 emergency admissions, or about 13,200 admissions per day. Nearly 40% of patients waited longer than four hours before being admitted or discharged. With increasing demand on the emergency services and increased pressure on acute wards, delays in information transfer and disconnected clinical systems represent a significant bottleneck. According to NHS England, over 40% of delays in acute admissions relate to missing or fragmented patient data, and/or poor interoperability between systems. The need for improved EHR Systems in Acute Care, to connect each step of a patient’s journey, triage-admission-discharge, has never been more urgent. CellmaEHR is the comprehensive, clinically intelligent solution to support patient flow, documentation, and diagnostics at speed, safety, and enable seamless integration to the NHS. CellmaEHR is the solution of choice for trusts who need to deliver coordinated, quality acute care. Aligned to the NHS Vision for Integrated, Connected, and Safer Care Cellma aligns with the NHS 10 Year Plan to support a digitally enabled, integrated, patient-centric model of care. Cellma interrogates data and people continuity between hospitals, to neighbourhood care, and virtual wards, to ensure every patient receives the same standard of care, whether this is at home, in their bed or in a hospital bed, wherever is appropriate for their needs. Cellma provides healthcare professionals with a single point of access to real time information, enabling timely clinical judgments and coordinated efforts from multidisciplinary teams. It is through the reduction of administrative burden and encouraging collaborative working relationships between acute and community settings, where Cellma fully exemplifies the NHS vision for connected, resilient, and efficient healthcare ecosystems. NHS and Global Standards, Integrations, and Datasets With NHS and international compliance at its core, CellmaEHR meets every mandated national, local, and global standard needed to support safe, interoperable and efficient delivery of acute care. National Digital & Clinical Safety Standards – Cellma complies with all essential UK and NHS digital safety frameworks: DCB0129 (manufacturer) and DCB0160 (deployment) for clinical risk management and assurance. Data Security and Protection Toolkit (DSPT), ISO 27001, Cyber Essentials, and UK GDPR for data protection and cybersecurity. Alignment with the NHS Data Protection Act 2018, NHS England Digital Clinical Safety Strategy, and DSP compliance requirements for NHS suppliers. These standards guarantee that every instance of CellmaEHR sustains clinical safety, operational resilience and confidentiality of patient data. Interoperability & NHS Integrations Cellma is designed to connect seamlessly across the entire NHS ecosystem, and it connects with: NHS Spine, GP Connect and Summary Care Record (SCR) for identity verification and access to key patient information. e-Referral Service (e-RS) for secure and direct management of referrals. Personal Demographics Service (PDS) for accurate identity management and demographic reconciliation. These connections ensure a constant flow of information between hospitals, neighbourhood care centres and virtual ward networks. This supports the overarching NHS vision for improved connected, continuous care. Clinical, Technical & Global Standards Cellma EHR facilitates compliance with a broad range of NHS and international interoperability standards so that hospitals can be confident of NHS compliance and connecting with international health services and research networks. NHS & UK Standards: Use FHIR UK Core, HL7 v2, DICOM, CDA/CCDA, and PRSB eDischarge specifications to exchange structured information. Use standard terminologies, such as SNOMED CT, ICD-10, LOINC, dm+d, and OPCS-4, to collect data consistently and in code. Reporting & National Datasets CellmaEHR supports easy statutory reporting and audit processes through automated, coded data extraction for NHS datasets, including: Hospital Episode Statistics (HES) and SUS (Secondary Uses Service) submissions. Care Quality Commission (CQC) notifications and incident reporting workflows. Infection control datasets, including HCAI surveillance and ICNARC for intensive care audit. National Hip Fracture Database, NCEPOD and mortality reviews for specialty reporting. Also, with connections to population analytics frameworks and FHIR Bulk Data export for research and performance monitoring. Global Healthcare Integration Built for global healthcare, enabling connected, patient-centred, and digital-first care anywhere in the world. Built with FHIR and HL7 standards for interoperability with global EHRs and healthcare IT systems. Fully compliant with GDPR, DSPT, and other international data protection frameworks. Connects with national health platforms and telehealth ecosystems worldwide. Scalable for healthcare providers, ministries of health, and private networks across multiple regions. Cellma also supports dataset mapping for ICU registries around the globe as well as WHO Global Health Observatory metrics and clinical trial data capture making it easy for hospitals to ensure they meet external audit and reporting needs, regardless of whether they are NHS related. CellmaEHR adheres to NHS and internationally recognised standards, interoperability protocols, and dataset integrations to guarantee full compliance, effective data sharing, and a connected digital ecosystem to improve clinical safety and operational efficiency in every aspect of care. How CellmaEHR Delivers Complete Solutions for Acute Care Admissions, Transfers & Discharges (ADT): Enables real-time visibility of patient admissions, transfers and discharges with live bed state visibility and NHS Number validation to reduce waiting times and improve the flow of patients from point of entry to discharge. Clinical Documentation & Decision Support: Supports structured ward-round notes, allergies, diagnosis, and treatment plan documentation with clinical decision support built in for sepsis detection, drug interactions, and renal dosing to enable safe and accurate documentation under pressure. AI-Enabled Functions Leverage predictive analytics for early warning alerts, resource forecasting, and readmission risk analysis. AI-powered triage and pattern recognition support proactive decision-making and operational efficiency. Voice-to-Text Documentation Enable clinicians to dictate notes directly into patient records, reducing administrative burden and improving accuracy through natural language processing (NLP). Observation Monitoring & ICU Integration: Integrates with monitoring systems to capture vital signs, NEWS2/EWS scores, and escalation alerts
EHR vs. EMR: How Cellma Delivers the Best of Both
Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Your browser does not support the audio tag. Table of Contents When discussing digital healthcare records, you may have heard the terms EHR (electronic health record) and EMR (electronic medical record) used interchangeably. At first glance, the difference seems so small, just a single letter, but that letter indicates a vast difference in the spectrum, intention, and patient care delivery. Across the world, adoption of digital software for patients records and other factors is steadily increasing. The World Health Organisation states that over 80–90% of hospitals and providers in higher-income nations are using some form of electronic record, however adoption is lower in middle- and low-income countries. Across the world, hundreds of hospitals and tens of thousands of hospital beds are being managed by EHR/EMR systems, although full interoperability is an ongoing process. In the UK, this digital shift is happening too; 94% of NHS trusts and 97% of GP practices are using an digital health records system in the form of either EHR or EMR, and over 12.25 million distinct users have control over their health records through the NHS App, all signalling a genuine move towards patient-centred, connected care and patient access. Recent studies highlight that AI-powered EHR solutions are significantly improving efficiency and patient safety across healthcare systems globally and in the UK. Around 90% of clinicians using AI-integrated EHRs report improved operational efficiency, with 60% saving up to four hours daily on documentation. Research also shows administrative overheads reduced by about 35%, while documentation time dropped from 4.3 to 1.8 hours per day with advanced digital systems. Hospitals using analytics-driven EHRs have achieved 10–20% savings in resource allocation, improved bed utilisation, and shorter wait times. On the safety front, EHR adoption has been linked to a 46% reduction in medication errors and up to 30% fewer diagnostic errors, while AI integration has further reduced medication error rates to nearly 2% and cut patient wait times by 13–17 minutes. Additionally, organisations leveraging regulatory analytics reported a 63% drop in compliance-related incidents, underscoring the dual benefit of AI in boosting efficiency and clinical safety. These adoption milestones are closely aligned with the NHS Long Term Plan (10-Year Plan), which places digital transformation at its centre. The plan aims for both the clinical and non-clinical activities within NHS trusts to be fully digitised by 2026, enabling clinicians to obtain accurate and real-time patient data across care settings and giving patients more control to have access to their own health records. The NHS 10-Year plan makes clear the importance of both EHRs and EMRs in delivering integrated, efficient and high-quality health care across the UK by focusing on interoperability, secure data sharing, and patient-centred digital services. Understanding EHR vs. EMR isn’t just about definitions; it’s about recognising how the right system can shape the future of healthcare delivery. What is EMR? An Electronic Medical Record (EMR) is a digital version of a patient’s chart within a single clinician’s office. Think of it as a modern version of all those big, thick folders being stocked away on clinic shelves. Key Features of EMRs: Records patient medical history, diagnoses, and treatments all within one practice. Provides digital charting, templates, and notes-taking options to allow for quicker documentation. Integrates with billing and coding to improve efficiency. Provides alerts and reminders for appointments or follow-ups. Advantages of EMR: Reduces paper records and errors. Saves time for clinicians by streamlining charting and workflow. Improves accuracy of treatment history within one practice. Enhances patient safety with prescription and treatment tracking. EMRs work best for smaller practices looking to digitise internal records, but the data typically doesn’t travel beyond the healthcare facility. What Is EHR? An Electronic Health Record (EHR), on the other hand, is much broader. An EHR is a comprehensive, digital version of a patient’s health information that is designed to be shared securely across multiple healthcare providers and organisations. This makes EHRs particularly valuable in today’s connected care environment. Features of EHRs: Comprehensive records, including demographics, lab results, imaging, etc. Interoperability: records available across hospitals, clinics, specialist care, national databases, and even patients. Patient portals help facilitate patient engagement and self-management. Advanced analytics and reporting for population health. Benefits of EHRs: Improve care coordination for multiple providers. A longitudinal view of a patient’s health history. Facilitate NHS interoperability and global interoperability standards. Improve efficiency and safety across healthcare organisations with e-prescribing, secure messaging, and mobile access. EHR vs. EMR: Key Differences Aspect EMR (Electronic Medical Record) EHR (Electronic Health Record) Scope Records within one practice Records across multiple providers & systems Data Sharing Limited or none Designed for interoperability Patient Focus Practice-centric Patient-centric, longitudinal Use Case Clinical workflow, billing, in-clinic use Coordinated care, telehealth, population health Access Providers in one clinic Providers, patients, and authorised stakeholders If EMR is practice-centric, EHR is patient-centric. This is the reason the EHR vs EMR distinction is relevant to today’s connected healthcare ecosystem. Cellma: The Best of Both Worlds At RioMed, we designed Cellma to bridge the gap in the EHR vs. EMR conversation by offering a single platform that adapts seamlessly to both needs. Whether a practice is looking for an EMR to manage patient records internally, or a healthcare system requires a fully interoperable EHR to connect providers, Cellma delivers a comprehensive, modular solution. What Makes Cellma Different: Modular Design for All Care Settings: Cellma is a comprehensive modular platform facilitating the entire patient journey across 30+ specialties. Key modules include: Patient Administration System (PAS) – admissions, scheduling, referrals and bed management. Electronic Patient Record (EPR) – clinical documentation, treatment histories, care plans and MDT collaboration. Document Management – secure access and retrieval of medical records, test results and clinical notes. E-Pharmacy & Prescribing – between prescription management, dispensing workflow and automated alerts of the risk of drug interactions. Laboratory & Imaging Integration – Cellma integrates with already established diagnostic systems. Theatre & Surgery Management – including surgical planning, theatre scheduling and reporting. Ward & Bed
Menopause Symptoms and Hormonal Balance: What to Know

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents Menopause is a natural phase in a woman’s life, marking the end of menstrual cycles and the hormonal changes that come with it. For many women, the transition can lead to various menopause symptoms which impact their physical, emotional, and mental health. Knowing what to expect, recognising the signs early, and how to manage them can help in easing the transition. With technology such as Cellmaflex, the experience is even easier. Navigating menopause has become significantly easier. You can book appointments with specialists online without waiting on hold during phone calls, access your complete medical history anytime, anywhere, and find nearby doctors, pharmacies, labs, or imaging centres quickly. In this blog, you will learn everything you need to know about menopause including what is menopause, menopause symptoms, health implications, lifestyle and medical management and how Cellmaflex will help to empower you to feel proactive and in control of your hormone health. Menopause – What You Need To Know about the Transition Menopause signifies the cessation of monthly periods and can happen anywhere from ages 45-55. Menopause is a natural process that occurs when the ovaries produce decreasing amounts of oestrogen and progesterone over the years. Then, as a side effect of this reduced ovarian function, a woman experiences changes in hormone levels. These hormone changes impact several systems of the body. Menopause occurs in all women at some time, but not every woman will have the same experience. Some women may experience very little interruption, while others will contend with significant impacts caused by menopause-related symptoms. According to the World Health Organisation (WHO), most women undergo menopause naturally between the ages of 45 and 55. In 2021, women aged 50 and over represented 26% of all women and girls around the world, an increase from 22% a decade previously, a fact that illustrates the increase in women entering menopause worldwide. This is relevant when studies show that in the Latin America and Caribbean region the prevalence of premature menopause is around 1.5% of women, and early menopause is approximately 1.9% of women, further illustrating the influence of age and region on menopause and its experience. Region Stats Latin America & Caribbean Prevalence of premature menopause is about 1.5%, and early menopause about 1.9%. (PMC) Latin America & Caribbean Median age at natural menopause: approximately 50 years. (PubMed) Latin America & Caribbean Mean age at menopause onset: around 44.4 years, slightly earlier than the global average. (PMC) Jamaica Around 130,000 women are menopausal, 76,200 perimenopausal, and 75,000 postmenopausal. (Jamaica Observer) The Phases of Menopause Menopause is not an immediate development; it occurs over time and involves various phases: Perimenopausal Period The perimenopausal period includes the time leading up to menopause where women may experience fluctuating hormonal levels, causing missed periods and symptoms like hot flashes and sleep problems. Women may also notice small changes in their mood as well as changes in their metabolism. Menopause You officially enter menopause when you have had an absence of menstrual periods for 12 months. At this stage, hormone levels have significantly decreased, and symptoms may worsen. Post menopause Post menopause begins after you have entered menopause and will last the remainder of your life. While some of your symptoms may diminish, health risks start to increase, such as increased chances of osteoporosis or heart disease, or changes in metabolism. Women can use Cellmaflex to schedule routine screenings, seek labs that are located near them, and track their health, using a preventative approach during this stage. Common Symptoms during Menopause Menopause typically accompanies physiological and psychological changes for women. Early recognition of common menopause symptoms can help you prepare to manage them. Some of the common ones include: Irregular periods or periods that are heavier or lighter than usual Hot flashes, also known as vasomotor symptoms (a sudden feeling of warmth that spreads over your body) Night sweats and/or cold flashes Vaginal dryness that causes discomfort during sex Urinary urgency (a pressing need to pee more frequently) Difficulty sleeping (insomnia) Emotional changes (irritability, mood swings or depression) Dry skin, dry eyes or dry mouth Worsening premenstrual syndrome (PMS) Breast tenderness Some people might also experience: Racing heart Headaches Joint and muscle aches and pains Changes in libido (sex drive) Difficulty concentrating or memory lapses (often temporary) Weight gain Hair loss or thinning Health Effects of Menopause While menopause symptoms themselves can be challenging, the hormonal changes can also increase long-term health risks: Osteoporosis: Less estrogen can mean thinner bones, increasing your fracture risk. It is important to monitor bone mineral density levels, and you can schedule a bone scan at a nearby imaging centre via Cellmaflex. Heart Disease: Lower estrogen can change your cardiovascular health and increase your risk of heart problems and strokes. You can book cardiology check-ups and monitor cholesterol and blood pressure via Cellmaflex. Metabolic Changes: You may easily gain weight, develop insulin sensitivity, or see changes to your cholesterol levels. You can also connect with endocrinologists, dietitians, and other specialists who work with hormones via Cellmaflex. Mental Health: Hormonal fluctuations can also exacerbate mood changes, anxiety, or depression. Managing menopause effectively involves a combination of lifestyle changes, medical treatments, and active follow-ups. A holistic approach enables a woman to decrease the severity of their symptoms, maintain long-term health, and improve their overall well-being. When to Seek Medical Attention You should seek medical attention if: Your symptoms are interfering with your daily life You are experiencing severe hot flashes or night sweats You have risk factors for osteoporosis, heart disease, and metabolic disorders It is always best to access care sooner rather than later. Use Cellmaflex to identify specialists, book urgent appointments online, and keep track of a complete medical history without the hassle. Lifestyle Changes Making small, but consistent changes to your daily routines can have a major impact: Balanced Diet: Eat calcium, vitamin D, and plant-based nutrients to promote bone health and preserve
Beyond Cervical Cancer Symptoms: A Guide to Women’s Health

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents Cervical cancer is an important global health issue for women, and early detection saves lives. Recognising the symptoms of cervical cancer and acting upon them with a timely evaluation with your medical professional can significantly affect how treatment will result. Being able to access care and treatment is a large contributing factor, but many women still forego screening or ignore early warning signs that make treatment challenging and reduce survival. With Cellmaflex, managing health is easier. Women can quickly book cervical screening appointments online without waiting on phone calls, access their complete medical history anytime, and find nearby trusted doctors, pharmacies, labs, or imaging centres instantly. In this blog, we will cover everything you need to know about cervical cancer – its definition, causes and risk factors, cervical cancer symptoms, complications, diagnosis, treatment options, prevention strategies, and how Cellmaflex can help women take control of their health effectively. What Is Cervical Cancer? Cervical cancer starts in the cervical cells, which line the cervix, the lower part of the uterus that connects to the vagina. In most cases, the normal cervical cells will change into abnormal cells as a result of a persistent infection with a high-risk HPV; this virus can remain in the body for years before the development of these abnormal cells. If abnormal cells are not detected and managed before they progress even further, they can invade deeper layers of the cervix and spread to neighbouring tissues or organs and become invasive cervical cancer. Cervical cancer remains a major global public health challenge. The World Health Organisation estimated around 660,000 cervical cancer cases and 350,000 deaths related to the disease in 2022. Cervical cancer makes up a considerable portion of the cancer cases and deaths in females in the Caribbean region. Cervical carcinoma accounts for about 13% of all diagnosed cancers in Caribbean women, and approximately 10.4% of cancer deaths in the region. The table below provides a snapshot of some Caribbean cervical cancer epidemiology estimates: Region / Country Cervical Cancer Stats Region of the Americas ~78,000 new cases annually; ~40,000 deaths annually Latin America & Caribbean Incidence: 15.1 per 100,000 women; Mortality: up to 18.3 per 100,000 Caribbean (overall) Screening coverage past 3 years: ~56%; HPV types 16 & 18 cause ~70% of cases North America Incidence: 6.4 per 100,000 women; Mortality: ≈2.2 per 100,000 PAHO 2030 targets 90% of girls vaccinated by age 15; 70% of women screened by ages 35 & 45; 90% of women with precancer/invasive cancer treated Causes & Risk Factors The dominant cause of cervical cancer is persistent infection with high-risk types of HPV, mainly types 16 & 18. Nonetheless, several other causes can increase the overall risk of developing cervical cancer, such as: Smoking, which harms cells in your cervix and negatively affects your immune response. A suppressed immune system (for example, due to HIV infection or the use of immunosuppressive agents). Long-term oral contraceptive use (greater than 5 years). Multiple full-term pregnancies or early first pregnancy. Family history of cervical cancer, which may indicate a genetic predisposition. Women can use Cellmaflex to track their medical and family history digitally, ensuring that risk factors are not overlooked during consultations. The platform’s ability to share health records securely with specialists also means care is more coordinated and personalised. Cervical Cancer Symptoms Recognising cervical cancer symptoms early can lead to better outcomes. Unfortunately, early stages often present no noticeable signs, which is why regular screening is essential. As the disease progresses, cervical cancer symptoms may include: Watery or bloody vaginal discharge that may be heavy and can have a foul odour Vaginal bleeding after sex, between menstrual periods or after menopause Pain during sex (dyspareunia) If cancer has spread to nearby tissues or organs, symptoms may include: Difficult or painful urination, sometimes with blood in your urine Diarrhoea, pain or bleeding from your rectum when pooping Fatigue, loss of weight and appetite A general feeling of illness Dull backache or swelling in your legs Pelvic/abdominal pain Complications If left untreated, cervical cancer can extend beyond the cervix to affect nearby organs such as the bladder, rectum, and pelvic walls. As the disease progresses, it may potentially spread to organs far away from its original location (e.g. the lungs, liver or bones), causing complications throughout many organ systems. Untreated, these secondary complications cause additional pain and suffering and have emotional and psychological consequences for patients and their families. Cervical cancer progression can lead to serious complications, including: Severe pelvic pain: Due to the growth of cervical tumours that can press against nerve endings and supportive tissues around the tumour. Kidney issues: If the ureters (tubes that connect the kidneys to the bladder) are blocked it can lead to hydronephrosis (swelling of one or both kidneys due to a buildup of urine) or obstruction and loss of kidney function, and ultimately renal failure. Heavy or persistent bleeding: Advanced cervical tumours can penetrate blood vessels in the cervix or uterus and lead to persistent medication-resistant chronic anaemia, and its subsequent fatigue. Bowel and bladder dysfunction: If the cancer spreads to organs adjacent to the cervix, patients may have bladder issues such as incontinence and haematuria (bloody urine), or rectal bleeding. Bone pain or fractures: If the tumour or metastases (cancer cells that have spread from a primary tumor to a different part of the body through the bloodstream or lymph system) spread to bones, patients will experience severe local pain and potential pathologic fractures. Respiratory problems: Lung metastases can lead to respiratory issues, such as breathlessness, a cough which may be persistent and/or dry, or pleural effusion (build-up of fluid in the lung cavity). Liver problems: Liver involvement can cause jaundice, nausea, and abdominal swelling. Lymphatic obstruction: Cancer spreading to pelvic lymph nodes may cause leg swelling (lymphedema). Emotional and psychological stressors: People with advanced cancer often do experience anxiety, fear of recurrence, depression, and other mental health
Delivering Joined Up Care for Ageing Population with Cellma

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Your browser does not support the audio tag. Table of Contents In the UK, unmet care needs for older adults remain substantial, around 2 million people aged 65+ require more care and support than they currently receive. Long NHS waits, and delayed hospital discharges are increasingly common. Hundreds of thousands are left without adequate support, often “stuck” in hospital while waiting for social care packages to be arranged at home. The health demands are immense, 75% of people aged 75+ live with multiple long-term conditions, increasing to 82% for those over 85. Even though the NHS Long Term Plan describes a vision for integrated support across the country, there is still widespread inconsistency, delays, and lengthy bureaucratic processes, siloed funding, and workforce development that remains uneven. Cellma, a fully integrated and future-facing EHR solution, closes the gap and specifically aligns with NHS goals for ageing well and care that is connected, online, and person-centred. aligning directly with NHS priorities for ageing well and delivering connected, person-centred care. The Current State of Joined-Up Care for Older People The NHS Long Term Plan describes a vision for integrated and community-based support; however, many areas currently face: Poorly coordinated services – hospitals, primary care, social services and voluntary sector all use different systems that are separate to each other, delaying coordination. Discharge delays – medically fit patients remain in hospital as a result of community and social care not being ready to accept them. Disjointed information sharing – key patient data is either lost between providers or duplicated. Limited rapid-response capability – services don’t have the ability to quickly mobilise teams in order to maintain clients and avoid readmissions. For an ageing population, these gaps mean slower recovery, avoidable hospital stays, and declining independence. How Cellma Powers True Joined-Up Care Cellma is more than an EHR, it’s a fully integrated digital health ecosystem designed to operationalise the NHS 10-Year Plan’s ambitions for connected, patient-centred care. Here is how it fits within the clinical workflow of joined-up care for older people: Hospital Discharge Planning The hospital clinician’s decision on discharge is instantly recorded in Cellma’s shared electronic health record. So, the day the patient is discharged, the community team, GP and social care providers receive notification, in real time, with no paper delays, to start care at home as soon as the person reaches home. Coordinated Care planning in the community Cellma provides a framework for planning home care and district nursing appointments, therapy appointments, voluntary services which can all be managed in one coordinated calendar. Post Hospital discharge assessments The initial and subsequent assessments can be added into Cellma which provides GP follow up, as a reminder. All notes, tests results and care plan updates can be accessed at once and in real time, by all health and care providers that the patient has given consent to. Live care plan and monitoring. If there is any change in the patient’s health status, the providers in the community can update the live care plan, viewable in real time by multi-disciplinary teams, reducing duplication and ensuring that the team can intervene quickly if needed. Rapid Response to urgent needs Rapid Response Teams have access to the most up to date medical records before arriving to see the patient, enabling them to provide informed and considered in-home care that prevents avoidable readmission. Care Coordination of Care across Settings Cellma enables care coordinators to manage the entire patient journey — from hospital admission to community-based follow-up — as a seamless digital record. Integrated Neighbourhood Teams Primary care, community health, local authorities and voluntary services access the same secure record and can more collaboratively deliver care for patients in their neighbourhoods. Population Level Frailty Management Cellma’s advanced analytics can help the organisation identify patients at risk of deterioration and engage in proactive frailty management to reduce dependency on hospital care in the community. Governance & Shared Outcomes Cellma’s reporting dashboards provide ICBs with their live clinical and demographic data and awareness of shared outcomes, e.g., reduction in frailty related admissions, speed of discharge times and independence at discharge rates. Virtual Wards & Early Discharge: The Future of Patient-Centred Care One of the NHS’s key strategies for joined-up care is the growing use of virtual wards. These allow clinically stable patients to continue receiving hospital-level monitoring and care at home, supported by digital tools and remote clinical teams. Equally important is the NHS drive for early discharge planning, where patients are safely discharged sooner, with a coordinated follow-up plan that ensures they do not return unnecessarily to hospital. This not only frees up hospital beds but also improves patient comfort and recovery in familiar surroundings. Momentum and Reach The NHS are scaling this rapidly, more than 10,000 virtual wards have been adopted in England, with over 15,000 planned as part of the NHS long term plan. Evidence suggests that virtual ward models employed in scale improve patient experience, enable safe discharge, and mitigate demand on hospital beds. Evidence of Effectiveness Evidence base supports their effectiveness. Evaluations highlight clear benefits: patients in virtual wards stay 3.07 days shorter than patients in hospital on average, and they can free up capacity while underlining the safety models proposed. In Southwest London, 74% of patients discharged to a virtual ward remained at home and not re-admitted into hospital, significant for it’s a real-world achievement! Caveats and Considerations Virtual wards aren’t universally designed to address everything, they can only improve care when delivered to appropriate patients, to recognise or reduce hospital-related complications, whilst the patient retains their independence at home. How Cellma Supports Virtual Wards & Early Discharge Integrated Workflows: Automated pathways from inpatient care to virtual ward and alerts with covered handovers. Real-time Monitoring: Insights derived from the automatic integration of wearable and at-home monitoring data for a proactive response. Care Coordination: Every member of the multidisciplinary team with access to and update capabilities within the record to ensure continuity of care in the home. Analytics
Improving Patient Experience in Dental Care with Cellma

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Your browser does not support the audio tag. Table of Contents The demand for quality dental care across the UK is at an all-time high, yet the sector faces mounting challenges. According to NHS statistics, only 40% of adults in England were seen by an NHS dentist in the last two years, down from 49% before the pandemic. While over 35 million courses of dental treatment were delivered in 2024/25, access remains uneven, especially in rural and deprived areas. Furthermore, oral health and disease conditions, including dental decay, periodontal disease, and late presentation due to covid backlogs continue to exert pressure on the service. These challenges underscore that there is an urgent need for advanced integrated electronic health record systems (EHR) that will manage dental workflows and integrated connections to wider healthcare pathways. CellmaEHR offers the solution, whether it be in hospitals, dental practices, or dental clinics, small or large, it offers a complete solution to improve the patient experience of dental care. Supporting the NHS 10-Year Plan Cellma is fully aligned with the NHS 10 Year Plan. Cellma provides support for digitally enabled primary healthcare, expanding community care in neighbourhood hubs, and aids in managing complex cases through the integration of a virtual ward. Cellma integrates with NHS Spine, GP Connect, NHS App and e-Referrals to create continuity of care for patients who move between dental and wider medical services. Cellma enables teams within a hospital or local clinics to cut waiting times, improve prevention, and provide safe dental care services all contributing directly to the NHS commitment to patient-centred care. Interoperability and compliance to NHS frameworks Cellma is built for seamless integration to NHS frameworks which allow dental practices, hospitals, and clinics to operate effectively and converge to local, regional, and national standards. Supporting national datasets, standards, and authentication frameworks provides a level of interoperability that supports reporting and patient safety whilst ensuring the right level of information is captured and accurately documented. Technical and Clinical Standards SNOMED CT – Standardised terminology with accurate clinical coding. HL7 and FHIR Protocols – Structured real-time data exchange across multiple NHS systems. DICOM – Ensures seamless integration of dental imaging and radiographs. PRSB Record Standards – Structured and interoperable patient records. NHS Number Integration – Ensures accuracy of patient identity across systems. NHS Integrations Spine/PDS (Personal Demographics Service) – Access to verified patient demographic information. NHS e-Referral Service (eRS) – Seamlessly refer patients to oral surgery, orthodontics and secondary care. EPS (Electronic Prescription Service) – Electronic prescription that is integrated directly into patient records. NHS Smartcard authentication – Secure access for clinicians in accordance with protocols from the NHS. NHS App Integration – Patients can view appointments, documents, and updates directly through the app. Incorporating these integrations and standards, Cellma provides assurance to dental practices that they are compliant, reducing administrative burden and being fully align Clinical Scope: Dental Conditions and Cellma’s Role Dental Condition How Cellma Assists Dental Caries & Tooth Decay Tracks progression through clinical notes, stores radiographs, records interventions, and automates recall reminders. Gum Disease & Periodontitis Integrates periodontal charting, lab test results, and structured notes for continuous monitoring and treatment planning. Oral Infections & Abscesses E-Pharmacy links with NHS EPS for quick prescriptions; secure documentation ensures safe antibiotic stewardship. Orthodontic Cases Imaging and document management modules support treatment plans, appliance tracking, and specialist referrals. Oral Cancers & Suspicious Lesions Structured templates for clinical findings, seamless referral pathways, and integration with neighbourhood care centres enable timely escalation. Dental Trauma (fractures, avulsions) Imaging integration and treatment workflow modules guide urgent care, documentation, and follow-up. Prosthodontics (dentures, crowns, bridges) Digital workflow supports lab integration, prosthetic tracking, and patient consent management. Cosmetic Dentistry (whitening, veneers) Clinical documentation ensures traceability, while patient portal supports treatment options and informed consent. Pediatric Dentistry Growth charts, fluoride treatment tracking, and recall reminders tailored for children’s oral health. Endodontic Cases (root canals) Imaging and treatment notes modules guide case complexity assessment and procedural documentation. Maxillofacial Surgery Referrals Cellma Connect (referral portal) ensures efficient transfer of radiographs, imaging, and notes to secondary care. Special Care Dentistry (patients with disabilities or comorbidities) Interoperability with hospital records and virtual ward integration supports multidisciplinary care. Preventive Care (fluoride varnish, sealants) Automated recall schedules, BI reporting for public health monitoring, and patient education via portal. Temporomandibular Joint Disorders (TMJD) Clinical notes, imaging records, and referral pathways for physiotherapy or surgical teams are captured within Cellma. Tackling Everyday Challenges with Cellma The dental workforce faces burnout, access pressures, and rising administrative loads. Cellma directly addresses these problems through its dedicated modules: Patient Admission and Scheduling (PAS): Reduces appointment booking errors, manages recalls, and balances urgent care slots. Electronic Patient Records (EPR): Offers a comprehensive clinical view of the patient, including treatment history, radiographs, and laboratory results. Document Management: Prepares, organises, and manages FP17 forms, safely stores patient records and consent documents and manages NHS reporting accurately. Laboratory and Imaging Integration: All dental images, blood tests, and microbiology reports can be linked and incorporated into collaborative decision making. E-Pharmacy: Electronic prescribing and seamless library management with integration to today’s EPS creates a smooth medication supply process. Communication: Access to care can be improved through secure messaging for patients to contact their provider, appointment reminders, and virtual appointments. Referral Portal (Cellma Connect): Patients can be referred into oral surgery, orthodontics, or secondary care correctly and according to NHS dataset requirements. Business Intelligence (BI) Reporting: Automatically provides compliance reporting, FP17 submissions and activity dashboards to relieve burdensome back-office functions. These modules ensure that hospitals, larger practices and small to medium sized practice or clinics can all reduce administration time and direct their energies to providing care, which ultimately improves patient experience in dental care settings. Data Security and Privacy Cellma is built with end-to-end encryption, GDPR compliance, DSP Toolkit certification, and Cyber Essentials Plus accreditation. Our system integrates fully with NHS datasets and standards; SNOMED CT, FHIR, HL7 and PRSB record structures.
Coronary Heart Disease Symptoms and Staying Heart-Healthy

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents Coronary heart disease (CHD) is the most prevalent form of heart disease and one of the leading causes of death in the world. Millions of individuals are diagnosed with CHD every year. CHD occurs when the coronary arteries, which provide the heart with oxygenated blood, become narrowed or blocked due to plaque build-up. Identifying the symptoms of CHD as early as possible can save lives, but many people can’t seek care due to busy work schedules or self-doubt about where to begin. This is why Cellmaflex can make a difference in your healthcare journey. With the ability to book appointments online, without ever needing to make a phone call, checking your entire medical history anytime, anywhere, and finding doctors, labs, imaging centres, and pharmacies in seconds, managing your heart health has never been easier. In this blog, we will define what is coronary heart disease, explore coronary heart disease symptoms, and identify major risk factors for the disease, diagnostic tests and prevention options, and discuss how Cellmaflex can help take control of your heart health proactively. What Is Coronary Heart Disease? Coronary heart disease (CHD), also known as ischemic heart disease, happens when the coronary arteries (blood vessels that carry oxygen-rich blood to the heart muscle) become narrowed or blocked with plaque. Plaque is a buildup of cholesterol, fat, calcium, and other substances that can be found in the inner lining of arteries, a process referred to as atherosclerosis. The buildup of plaque reduces blood flow, which restricts the heart’s access to the oxygen it requires to function properly. If left unchecked, CHD can lead to angina (chest pain), heart attacks, arrhythmias, or heart failure. In many cases, the first warning of CHD may be a heart attack, which is why it is important to monitor symptoms and risk factors for coronary heart disease. According to WHO, globally, coronary heart disease (CHD) caused approximately 9 million deaths in 2021, making it the single biggest killer worldwide. In 2022, an estimated 315 million people were living with CHD globally, including roughly 145 million men and 110 million women. WHO stated that cardiovascular diseases (CVDs), a broader category that includes CHD, caused an estimated 19.8 million deaths in 2022, representing about 32% of all global deaths. According to the Pan American Health Organization (PAHO), cardiovascular diseases (CVDs) remain the leading cause of death in the Americas, claiming over 2 million lives annually. In 2021, the age-standardized CVD mortality rates declined by 29.8% from 208.0 deaths per 100,000 population in 2000 to 146.1 deaths per 100,000 population in 2021. However, these rates vary significantly across countries, with Haiti having the highest rate at 427.7 deaths per 100,000 population. Country/Territory CVD Mortality Rate (per 100,000) Haiti 427.7 Dominican Republic 199.0 Jamaica 221.0 Trinidad and Tobago 193.0 Barbados 180.0 Saint Lucia 210.0 Saint Vincent and the Grenadines 215.0 Grenada 220.0 Saint Kitts and Nevis 230.0 Antigua and Barbuda 240.0 Taking care of your heart health is easier than ever with Cellmaflex. You can: – Find cardiologists and other specialists in your area – Book in-person or online appointments and diagnostic testing – Review your entire medical record to track your heart health trends – Coordinate care with labs, imaging, and pharmacies – Patients can do all these activities on their mobile devices in few taps! Coronary Heart Disease Symptoms Understanding the warning signs or coronary heart disease symptoms is important. Some patients have clear symptoms, while other patients are asymptomatic until a serious cardiac event arises. Here is a guide of what to look for: Chest Pain or Discomfort (Angina) Angina is the hallmark symptom of CHD. Patients often describe the sensation as pressure, squeezing, fullness, or tightness and may experience discomfort in the arms, shoulders, neck, jaw, or back. Usually, in the context of angina, the sensation rises with either an increase in physical activity or an increase in emotional stress when the heart requires more oxygen than the narrowed arteries can deliver. Shortness of Breath Reduced blood flow can impair the heart’s ability to pump efficiently, causing fluid buildup in the lungs and resulting in difficulty breathing, even during everyday activities Fatigue or Weakness If you are experiencing prolonged fatigue, it may be indicating that the heart is not receiving adequate oxygenated blood to ensure adequate bodily function. Heart Palpitations A heartbeat that is irregular or has an unusually fast rhythm can be a product of coronary arteries that may be unwell. Silent Symptoms Some individuals will have no symptoms at all until they experience a heart attack or sudden cardiac event: This is why a regime of routine monitoring and preventive health is crucial for this group of people. Key Risk Factors Some factors raise the chance of developing coronary heart disease. Understanding and managing the risks is important: High cholesterol levels and high blood pressure: Excess cholesterol can form plaques, narrowing arteries, while high blood pressure causes damage to arterial walls. Smoking and excessive alcohol: Both increase plaque formation and are detrimental to cardiovascular function Diabetes: High blood sugar damages blood vessels and increases the risk of CHD. Obesity and poor nutrition: Diets that are high in saturated fat, refined sugar, and processed foods contribute to plaque build-up. Physical Inactivity: A sedentary lifestyle weakens the heart and reduces circulation efficiency, increasing the risk of plaque buildup and coronary heart disease. Family history of heart disease: Genetics may contribute to the potential for developing CHD. With Cellmaflex, you will be empowered to address these risk factors. You can find dietitians, fitness professionals, and wellness clinics in your area, schedule follow-ups, and maintain records of key health indicators such as cholesterol, blood pressure, and blood sugar, all in one user-defined, user-friendly, simple-to-use digital health platform. Prevention and Management Engaging in preventive lifestyle practices and regular self-management can help prevent or manage coronary heart disease. Eat a Heart-Healthy Diet: Emphasise fruits, vegetables, whole grains, lean protein, and healthy fats while minimising processed foods and
The Role of CellmaEHR in Neonatal and Paediatrics: Safer and Smarter Care

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Your browser does not support the audio tag. Table of Contents Newborn and child healthcare in the UK is facing increasing pressures. According to the Office for National Statistics (ONS, 2023), the neonatal mortality rate in England and Wales stands at 3.0 deaths per 1,000 live births, while infant mortality remains at 3.9 per 1,000 live births. Despite advancements in clinical practice, around 70% to 80% of all infant deaths occur during the neonatal period. Babies born before 24 weeks though fewer than 0.1% of births, accounted for 37.4% of neonatal deaths, with a mortality rate of 782.2 per 1,000 live births in this group. The National Child Mortality Database (2024) reported a child mortality rate of 29.8 deaths per 100,000 among children aged 0–17 years, underscoring persistent challenges in paediatric healthcare delivery. Hospital pressures also remain high, with over 829,000 emergency admissions of children under 18 recorded across the UK in 2023–24. These figures reflect the ongoing demand for efficient, integrated systems to manage neonatal and paediatric care, where accurate data, timely interventions, and cross-departmental communication are crucial for improving outcomes. Aligned with the NHS 10 Year Plan for virtual wards and neighbourhood care teams the CellmaEHR provides neonatal and paediatric care outside the four walls of a hospital. Cellma brings together maternal-baby records, NICU flowsheets, and outpatient paediatric workflows to create continuity of care across multiple care settings. The platform supports “structured” data capture for national datasets and reporting e.g., MSDS, Neonatal Data Set (NNRD), HES/SUS datasets, and helps to enable interoperability via the FHIR UK Core and SNOMED CT standards. For hospitals striving to provide fully integrated, safer care and meeting NHS aspirations, CellmaEHR in neonatal and paediatrics is not simply a clinical tool; it is a key partner in the delivery of care. Integrations and Standards Utilised by Cellma CellmaEHR has been developed to ensure that all aspects comply with UK healthcare standards, while integrating easily with existing hospital systems: National Standards & Terminologies: FHIR UK Core for interoperability, SNOMED CT for clinical terminology, LOINC for labs, ICD-10/OPCS for coding. NHS Spine / GP Connect: Enabling access to summary patient data, patient demographics and coordination of discharge. Electronic Prescription Service (EPS): Dosing workflows for child discharge prescriptions. Laboratory and Imaging Systems: Bidirectional integration with laboratory information systems (LIS), picture archiving and communication systems (PACS), radiology information systems (RIS) and any laboratory or imaging systems. Pharmacy and Blood Bank Systems: Drug reconciliations, neonatal drug library, medications tracked through infusion pumps, tracked by batches, or lots. Device and Bedside Integration: Receipt of real time device data from monitoring equipment, ventilators and infusion pumps using HL7 or FHIR streams. Public Health & Screening Services: Automatically capturing and reporting newborn bloodspot screening, hearing screening, and retinopathy of prematurity (ROP) screening. Data submissions & research: MSDS, Neonatal Data Set (NNRD), HES/SUS, & ONS reporting, including field-level validation. Security & privacy compliance: the GDPR, Data Security & Protection Toolkit (DSPT), & Caldicott principles and processes including role-based access, encryption, audit logs, & pseudonymisation for secondary research purpose. Parent and Care Coordination Portals: Regulated access to the records & assessments with consent to comply with the neonatal aspects. Through these specifications and integrations, CellmaEHR provides trustworthy, secure, and future-proof Electronic Health Records for neonates and paediatrics, supporting a single care ecosystem for modern hospitals and the NHS. Clinical Scope: Neonatal and Paediatric Care Population / Area Data & Features Neonates (delivery room, SCBU, NICU, transitional care) – Gestational & corrected age tracking, birth weight, APGAR scores, maternal linkage- Hourly/daily vitals, ventilator parameters, oxygen/CPAP settings, nutrition management (breastmilk, donor milk, parenteral nutrition)- Weight-based medication dosing with pump/infusion integration, transfusion tracking, lab results integration- Screening: bloodspot, hearing, congenital heart, ROP exams Paediatrics (children & young people, outpatient, ward, PICU) – Growth & development tracking (birth to 18 years), vaccination history, allergy documentation, PEWS scoring- Structured lab & imaging orders with SNOMED CT-coded problem lists- Safeguarding & social risk flags Challenges Addressed – Fragmented systems, data gaps, and alert fatigue- Resolved by Cellma EHR through maternal–baby linkage, device feeds, weight-based dosing alerts, and configurable clinical decision support tailored to neonatal and paediatric physiology Core Features of CellmaEHR Cellma’s platform can address the clinical, operational and compliance challenges within hospitals: Clinical Documentation and Flowsheets: Minute to minute neonatal flowsheets and paediatric ward templates with structured problem lists and configurable order sets. Drug Interaction: Weight and age-driven medication dosing engine, unique drug library for neonates, barcode medication administration (BCMA), and infusion pump interoperability. Order Entry & Results: Computerised Physician Order Entry (CPOE) that integrates with lab, imaging, and microbiology results. Device & Bedside Integration: Providing accurate documentation with live HL7/FHIR feeds from monitors, ventilators, and infusion pumps. Care Coordination: Involving maternal-baby links, discharge messaging to GPs/health visitors, and parental portals that can only be accessed through consent. Dashboards & Analytics: Including live NICU occupancy, tracking of ventilators, PEWS escalation for sick babies and planned extracts to send data to NNRD, HR-XML, HES/SUS, and MSDS. AI & NLP Intelligence in Cellma – Cellma uses AI and NLP to analyse clinical notes, detect risks early, and support accurate decision-making in neonatal and paediatric care. By linking all these modules together, Cellma alleviates burdensome administration, improves data quality for audits, and maximises staff attention on patients rather than paperwork. Security and compliance Cellma complies with all UK legal and NHS obligations, including GDPR compliance, DSP Toolkit compliance, and adopting the Caldicott principles. Sensitive neonatal and paediatric data are protected, with end-to-end encryption, role-based access control, audit record with logs, and multi-factor authentication. Cellma also uses pseudonymisation and secure extraction tools for safe secondary use of information for research and benchmarking. Why choosing Cellma is the right choice No matter if you are a NICU nurse or paediatric consultant, efficiency for staff and safety for patients is the most important aspect. CellmaEHR: Helps you spend less time calculating doses or retrieving historical records. Allows you to report accurately to national datasets. Easily integrates into virtual wards and neighbourhood care centres. Provides
Breast Cancer Symptoms, Diagnosis, and Treatment: What You Should Know
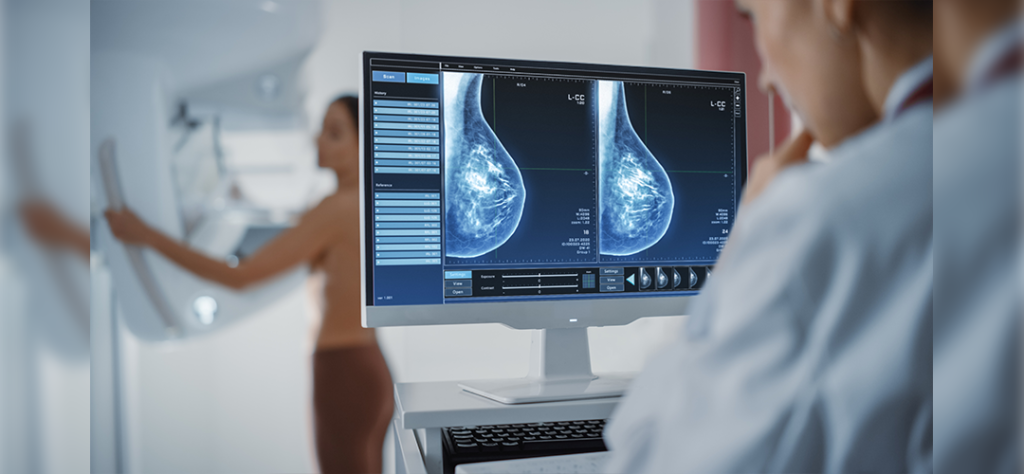
Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents Hearing the words “you might have breast cancer” is one of the most overwhelming moments in a woman’s life. For many, it may start with noticing a small lump, a change in shape, or swelling, or a persistent pain that just feels “different.” The uncertainty, anxiety, and fear that follow can feel paralysing. Breast cancer not only affects the body but affects a woman’s emotional health, family life, daily routines, and way of life. With tools like Cellmaflex, managing health has become far more convenient. Women no longer need to wait endlessly on phone lines to book medical appointments. Instead, they can easily book an appointment online, access their medical record whenever they want, and search a doctor, pharmacy, lab, or imaging centre in their area in a matter of seconds. In this blog, we will cover everything you need to know about breast cancer, what is it, types, causes, breast cancer symptoms, complications, diagnosis, treatment, and how Cellmaflex helps promote better access to healthcare services and monitoring for patients. What Is Breast Cancer? Breast cancer occurs when abnormal breast cells begin growing uncontrollably, forming a tumour. These tumours may be benign (non-cancerous) or malignant (cancerous). Malignant tumours can invade surrounding tissues and may spread (metastasize) to other parts of the body if untreated. Recognising breast cancer symptoms early plays a pivotal role in stopping the disease from progressing. Cellmaflex plays a supportive role here by allowing women to keep a digital record of their medical history, imaging, and test results, making it easier for both patients and doctors to identify changes in breast health over time. According to the World Health Organization (WHO), breast cancer is the most common cancer among women worldwide. In 2022, there were an estimated 2.3 million women diagnosed with breast cancer and 670,000 deaths globally. Early detection saves lives, and while this is true for many women, many still wait to seek medical help until the symptoms of breast cancer have progressed. This often complicates treatment and worsens outcomes for women. Caribbean & Trinidad & Tobago Breast Cancer Statistics Statistic Detail Breast cancer is the leading cancer overall in Trinidad & Tobago Of 3,095 registered breast cancer cases in that period, it accounted for 17.6% of all cancers, and among women, it accounted for 33.1%. Incidence & mortality rates in T&T For women, the age-standardized incidence rate for breast cancer is 46.6 per 100,000; representing ~31.6% of female cancer cases. Survival rate in T&T The 5-year breast cancer survival rate is about 74.3%, with a recurrence-free survival rate of 56.4%. Trends in Jamaica In Jamaica, breast cancer made up more than one out of every three cancer diagnoses in women; ~1,208 new cases in 2020 (up from 974 in 2018). Mortality in Jamaica The death rate from breast cancer has increased from about 56.8 to 66.9 per 100,000 women over recent years. The case fatality (percentage of diagnosed women who die) ranges between 41% to 51%. Incidence & mortality across Caribbean countries • Haiti: incidence ~22/100,000; mortality ~11.5/100,000. • Bahamas: incidence ~98.9/100,000; mortality ~26.3/100,000. Age of peak incidence In most Caribbean countries, peak incidence of breast cancer is in the 65-69 age group, or sometimes later (70-74). Some countries have secondary peaks under age 60. Breast cancer types 1. Non-invasive (in situ) cancers The most common is ductal carcinoma in situ (DCIS), where there are abnormal cells in the lining of a breast duct, but it does not spread to the tissue nearby. DCIS is not life-threatening in the immediate sense, but it can lead to an increased risk of invasive breast cancer later. 2. Invasive cancers Invasive ductal carcinoma (IDC): The most common form of breast cancer. Starting in milk ducts then invading surrounding breast tissue. Invasive lobular carcinoma (ILC): Begins in lobules (glands that produce milk), often grows in a less defined pattern making it more difficult to identify. 3. Other types There are some rare but aggressive forms of breast cancer, such as inflammatory breast cancer – which causes red and inflamed tissue – and triple-negative breast cancer, which does not respond to hormonal therapies, which usually require chemotherapy. Causes & Risks Although there are multiple risk factors that increase the risk of breast cancer, the cause is often not clear. Age: More common among women aged over 50. Genetics: Hereditary mutations in genes such as BRCA1 and BRCA2 greatly increase susceptibility. Lifestyle factors: Obesity, sedentary lifestyle, alcohol consumption, and smoking. Hormonal influences: Early menstruation, late menopause, and long-term hormone replacement therapy. Cellmaflex can help women at higher risk by making it easier to schedule regular screenings, track family history, and access imaging or lab test results in one place. Breast Cancer Symptoms Recognising breast cancer symptoms early is essential. Signs include: A lump or thickening in the breast or underarm. Changes in breast size or shape. Skin changes such as dimpling, redness, or swelling. Nipple discharge (other than breast milk) or inversion. Persistent pain in one part of the breast. Should you observe any of the breast cancer symptoms it would be judicious to reach out to your healthcare provider promptly. Cellmaflex can help you with this process by allowing you to book your appointment online and find the closest imaging centre for your mammogram or ultrasound. Complications When breast cancer is untreated, it can cause significant complications, such as: Bone metastases – leading to fractures, pain, and restricted movement. (Metastases: are secondary tumors formed by the spread of cancer cells from a primary tumor to a distant part of the body through the bloodstream or lymph system.) Metastasis to the liver – jaundice (yellow eyes/skin), or abdominal swelling, and liver failure. Metastasis to the lung – chronic cough, shortness of breath, or chest pain. Brain metastases – causing headaches, seizures, changes in vision, or neurological deficits. Recognising breast cancer symptoms early and obtaining medical care as soon as possible is important for preventing the above complications. Diagnosis Early
CellmaEHR: Leading Oncology Clinical Management Software for Cancer Care

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Your browser does not support the audio tag. Table of Contents Cancer prevalence has risen from nearly 3 million in 2020 to almost 3.5 million in 2025 and is expected to keep increasing. The demand for cancer care in the UK is at an unprecedented level. In 2025, there will be over 400,000 new cases for cancer, or roughly 1,100 people diagnosed per day. About 45.5% diagnosed in England (for those with known stage) are found at Stage 3 or 4. Breast, prostate, lung, and bowel cancers together account for over 50% of all new cancer cases. The NHS Long Term Plan aims to reach 75% of cancers diagnosed at early stage (1 or 2) by 2028. While survival rates do continue to rise, the sheer volume of cancer incidence and complexity of care pathways has markedly increased work engagement for oncology teams. From referrals, diagnostics, treatment planning, multidisciplinary meetings and survivorship care, administrative work demands have absorbed precious time that could be used more productively with patient care. This is where CellmaEHR steps in. Designed to reduce the oncology department administrative burden while aligning with all NHS integrations and standards. CellmaEHR, an oncology clinical management software aligns with NHS integrations, datasets, and the objectives of the NHS 10 Year Plan. Cellma reduces administrative burden while enabling better care coordination, neighbourhood-based support for early detection, and integration with modern models of care such as virtual wards. NHS Standards and Integrations Supported by Cellma Cellma adheres with and integrates fully with the complete suite of NHS datasets and guidelines for oncology-related data compliance and continuity of cancer pathways: Activity Datasets: Cancer Waiting Times (CWT), Hospital Episode Statistics (HES), Systemic Anti-Cancer Therapy (SACT), Radiotherapy Dataset (RTDS). Outcome Datasets: National Cancer Registration and Analysis Service (NCRAS), Office for National Statistics (ONS), National Cancer Audits, and Cancer Patient Experience Survey (CPES). Standards & Compliance: Fully compatible with NHS Spine services, GP systems, NHS App, Neighbourhood Care Records, and Virtual Ward Integration, while supporting HL7, FHIR, and CQC requirements for interoperability and data governance. Interoperability & Technical Standards: Cellma is HL7 v2/v3 message, FHIR APIs, DICOM for imaging, SNOMED CT terminology, ICD-10/11 coding, Read Codes and OPCS-4 procedure codes enabled, facilitating the consistent transfer and reporting of data across the complete oncology care pathway. By using these data sets, Cellma reduces duplication, allows for reporting to be automated, and allows oncology departments to demonstrate they are meeting national standards for performance with no additional administrative burden on the oncology department. Clinical Scope: The Management of Oncology Conditions with Cellma Oncology is not a condition, but a spectrum of cancers and associated issues. The most common cancers in the UK – breast, lung, prostate, and bowel, account for over half of all cases. Beyond these, oncology care must manage rare cancers, paediatric cancers, haematological malignancies, and acute oncology presentations such as neutropenic sepsis or spinal cord compression. Cellma facilitates the complete clinical process: Referral and Diagnosis: Oversees urgent GP referrals in the 2-week wait process, interacts with imaging and pathology systems, and helps automate the sharing of results. Multidisciplinary Team (MDT) Management: Provides structured MDT templates in which oncologists, radiologists, and surgeons can collaboratively document decisions in real time. Treatment Planning and Monitoring: Supports systemic anti-cancer therapy (chemotherapy, targeted therapy, immunotherapy), radiotherapy and surgical oncology. Acute Oncology Services: Records emergency admissions, and treatment complications, and ensures an expedient escalation. Follow-up & Survivorship: Generates automated end-of-treatment summaries, follow-up schedules, and survivorship care plans. Cellma digitises and coordinates these stages in a manner that maintains absolute clinical meaningfulness and reduces the complexity of the Oncology department’s administration associated with paper records, typing the same information in multiple systems, and broken communication. Key Features of Cellma EHR for Oncology Care Oncology departments face a unique set of administrative burdens: high referral volumes, complex treatment regimens, constant reporting to national datasets, and the coordination of MDTs. Cellma offers a solution to these issues in a clinically rich fully integrated platform: Electronic Patient Record (EPR): Gathers all oncology data (referrals, test results, imaging, treatment summaries) into a single locus of easily accessible information. This prevents redundancy and enables continuity of care across various providers. Patient Admission and Scheduling (PAS): Automates scheduling for diagnostics, consultations, and treatments, reducing appointment backlogs and cutting waiting times. Document Management: Digitises consent forms, MDT outcomes, and treatment plans, ensuring fast retrieval and compliance with NHS audits. Laboratory and Imaging Integrations: Integrates with pathology, radiology, and genomic testing platforms which are essential for accurate staging of cancer and personalised therapy. Pharmacy and Chemotherapy Management: Monitors all aspects of systemic anti-cancer therapy prescriptions for each patient, the dosage adjustment and side-effect management allowing minimising all medication errors and administration workload burden from therapy management. Theatre Management: Manages all aspects of surgical oncology scheduling and consumables so that cancer surgery is not delayed. Business Intelligence and Reporting: Provides automated CWT, SACT submissions, RTDS submissions, and NCRAS submissions all of which are useful to expedite manual reporting which causes delays in the Oncology Department Administration. Each module is designed to alleviate a particular pain point – whether it is delays in referral, data that has been missed by the MDT, or whether it is just the manual workload through reporting. With Cellma oncology teams spend less time on admin and more time on the patient-centred care. Security and Compliance in Oncology Care Oncology data is amongst some of the most sensitive patient health data in healthcare. To create confidentiality and trust for patients Cellma uses: Controls using role-based access and authorisation, preventing unauthorised access. End-to-end encryption of all data, in transit and at rest. Compliance with GDPR, NHS Digital standards and ISO certifications. Audit trails to provide accountability and transparency of all clinical and administrative actions. By implementing these, Cellma protects oncology data while reducing the risk of exposure to compliance breaches which only serve to increase the oncology department administrative burden. Oncology teams across the UK are facing high demand, increased complexity, and additional administrative requirements. Cellma EHR is a clinically robust


