Smarter EHR for the General Medicine Department with Cellma

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents In today’s fast-paced healthcare landscape, the General Medicine department is under unprecedented pressure. With rising patient volumes, complex comorbidities, and a growing need for coordinated care across specialties, the demand for a robust and efficient Electronic Health Record (EHR) system is more crucial than ever. In 2023–24, NHS England reported over 41 million outpatient attendances, with over 9.6 million first-time appointments and 2.9 million remote consultations, a large proportion under General Medicine departments. Whether managing frailty in elderly patients or diagnosing unexplained systemic symptoms, General Medicine is the backbone of acute and internal care. Enter Cellma, a fully integrated, NHS-aligned EHR platform designed to meet the clinical and administrative complexities of the General Medicine department. In addition to high patient volumes and acute admissions, General Medicine departments across the UK are managing an increasing burden of chronic diseases. According to data from over 12 million patients in NHS primary care, approximately 21% of adults are living with obesity, while 17% are diagnosed with depression. Hypertension affects around 15–18% of patients, asthma around 15%, and anxiety disorders over 13%. Musculoskeletal conditions like osteoarthritis impact 11–12%, while diabetes mellitus and chronic kidney disease are present in around 5% of cases each. Coronary heart disease affects another 5%, and COPD is recorded in approximately 2.7% of adult patients. With such a wide range of overlapping conditions, the clinical complexity faced by General Medicine departments is immense and Cellma is built to support every step of that journey. NHS Integration and Clinical Compliance Cellma is designed to align with all NHS integration standards and clinical guidelines, ensuring seamless functionality within public health systems. Cellma supports: NHS e-Referral Service (e-RS) for outpatient and urgent care bookings Summary Care Record (SCR) access Electronic Prescription Service (EPS) GP Connect for real-time data exchange with general practice HL7, DICOM, and FHIR standards for lab, imaging, and third-party interoperability NHS England’s Same Day Emergency Care (SDEC) framework Compliance with NHS England’s 14-hour review target for emergency admissions This ensures that Cellma not only improves clinical care delivery but also adheres to national performance targets and interoperability mandates, critical for the General Medicine department. Clinical Conditions Managed in General Medicine and How Cellma Assists Clinical Condition How Cellma Assists the General Medicine Department Heart Failure (HFrEF, HFpEF, HFmrEF) – Integration with BNP, ECG, and echocardiography for diagnosis – Structured documentation for NYHA class and daily fluid balance – ePrescribing modules for ACE inhibitors, beta blockers, and diuretics – Automated alerts for renal function monitoring – Heart failure nurse referrals and follow-up scheduling Chronic Obstructive Pulmonary Disease (COPD) – Real-time integration with pulse oximetry and ABG values – Spirometry result logging and GOLD classification templates – Oxygen therapy protocols and long-term home oxygen alerts – Exacerbation tracking and respiratory MDT referrals – Smoking cessation counselling and pulmonary rehab scheduling Ischaemic Heart Disease & Hypertension – ECG integration with immediate access to reports – QRISK2 calculators and statin eligibility prompts – Automated tracking of BP readings and antihypertensive therapies – ePrescribing tools with drug interaction alerts – Cross-specialty referral to cardiology when indicated Diabetes Mellitus (Type 1 & 2) – HbA1c trends and insulin titration dashboards – Alerts for annual foot exams and retinopathy referrals – Renal function monitoring (eGFR, ACR) integrated with care plans – Diabetes-specific care pathways including dietician and podiatry referrals – TTOs and discharge planning including diabetes nurse input Chronic Kidney Disease (CKD) – eGFR tracking with automated staging alerts – Fluid restriction and electrolyte replacement protocols – Medication safety alerts (e.g., nephrotoxic drugs) – Renal dietician and nephrology referral pathways – Coordination with dialysis planning and transplant units Pneumonia & Sepsis – CURB-65 scoring tool embedded in the clerking template – Sepsis 6 bundle checklist with timestamped action logs – Escalation alerts based on NEWS2 and vitals – Documentation of antimicrobial stewardship and response monitoring – Critical care referral and sepsis MDT documentation support Falls, Delirium & Frailty Syndromes – Frailty Index and Rockwood scoring tools – 4AT screening for delirium with behavioural tracking – Falls risk assessments and PT/OT referrals – Integrated MDT forms for rehab and care home planning – Advance care planning (DNAR, TEP) and community liaison Multisystem Syndromes (e.g. Vasculitis, PUO, Lupus) – Complex case tracking with symptom timelines and diagnostic flows – Auto-flagging of abnormal labs (CRP, ANA, ESR, cultures) – Integration of biopsy results and second opinions via document management – MDT discussion logs with input from rheumatology, neurology, ID – Custom templates for ongoing immunosuppressive therapy and monitoring Tackling the Real Challenges of General Medicine with Cellma 1. High Patient Flow Management General Medicine is often the first point of care for emergency admissions. Cellma supports: Streamlined Patient Registration & Triage at the AMU or MAU Structured Clerking Templates for rapid and complete documentation Queue & Bed Management Dashboards for real-time tracking Integration with early warning scores and escalation pathways 2. Time-Pressured Documentation Doctors frequently lose time creating discharge summaries and chasing investigations. Cellma offers: Auto-populated eDischarge Summaries with coded diagnoses, meds, investigations, and follow-up Investigation Tracking Panels that flag pending and urgent results Speech-to-text documentation tools for hands-free entries Built-in clinical calculators (CHA₂DS₂-VASc, CURB-65, Wells Score) 3. Multidisciplinary Coordination Delayed transfers due to social care gaps can block hospital flow. Cellma connects the entire care ecosystem by: Including Social Workers, Occupational Therapists, and Physios in the MDT interface Enabling shared care plans with Community Services and Virtual Ward Teams Allowing GP handovers with attached documents, TTOs, and alerts With Cellma, the General Medicine department can avoid unnecessary readmissions by ensuring patients are discharged with appropriate community-based support. Comprehensive Modules Supporting General Medicine Cellma delivers an end-to-end ecosystem that supports the entire care continuum: EHR & Clinical Notes: Custom templates for clerking, daily reviews, MDT meetings, and care plans Patient Administration System (PAS): Manages referrals, ward transfers, and discharge scheduling Laboratory Integration: Auto-imports bloods, urine, and microbiology results Imaging Integration: DICOM-compatible for instant access to
Your Guide to COPD Risk Factors, Symptoms, and Managing the Condition

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents Chronic Obstructive Pulmonary Disease (COPD) is a progressive lung condition that makes breathing difficult over time. It includes chronic bronchitis and emphysema, both of which cause lasting damage to the lungs. As one of the leading causes of death globally, COPD affects millions and puts a significant strain on patients and healthcare systems. Early recognition and management are key to better outcomes. Managing a chronic condition like COPD doesn’t have to feel overwhelming. Whether you’re a patient, caregiver, or clinician, Cellmaflex supports you at every stage, allowing users to book online appointments without phone calls, access their medical history anytime and anywhere, and find nearby doctors, labs, imaging centres, and pharmacies. A single digital platform designed to make your COPD care easier, helping you stay informed, engaged, and proactive. In this blog, we will get into what COPD is, global impact of COPD, significant COPD risk factors, symptoms, diagnosis, and treatment. We will also take a look at prevention and when to ask for help, as well as how Cellmaflex supports all aspects of your COPD care journey. Why Does COPD Demand Our Attention COPD is a progressive and terminal lung disease that is distinguished by a chronic inflammatory response in the lungs and persistent limitation of airflow. It’s not simply a ‘smoker’s cough’. The WHO over 3.3 million deaths globally were attributable to COPD in 2019, making it the third leading cause of death worldwide. It is estimated that COPD affects more than 390 million people globally, with prevalence rates continuing to rise, particularly in low- and middle-income countries where underdiagnosis is common. Notably, over 90% of COPD-related deaths occur in these regions, driven by factors such as air pollution, biomass fuel exposure, and limited access to healthcare. In some areas, studies estimate that up to 1 in 5 adults over age 40 may be living with undiagnosed COPD. What is COPD? Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. The major clinical entities that form the definition of COPD are: Chronic bronchitis: long term inflammation of the bronchi with daily cough and sputum production. Emphysema: destruction of the walls of the air sacs (alveoli) that cause air trapping (dead space), impaired gas exchange and reduced elastic recoil of the lung. Pathophysiology: the underlying mechanism of COPD is chronic airway and alveolar inflammation, based on an irritant (predominantly cigarette smoke) exposure. With time, it results in: Goblet cell hyperplasia and mucus hyperproduction Loss of cilia and decreased mucociliary clearance Bronchial wall thickening and narrowing Alveolar destruction (emphysema) Pulmonary vascular remodelling The result is airflow limitation that is not fully reversible, distinguishing COPD from asthma. Pulmonary function deteriorates progressively, eventually leading to respiratory failure. Who Is at Risk? Understanding COPD Risk Factors Knowing the COPD risk factors is essential to prevent or delay disease onset. While smoking remains the most significant factor, COPD can and does occur in non-smokers too. Smoking (Primary Risk Factor) Tobacco smoke is responsible for up to 70% of COPD cases in high-income countries. Both current and former smokers are at risk. Passive smoke exposure can also contribute, especially in children. Environmental and Occupational Exposures Air pollution, biomass fuel smoke, and second-hand smoke are major concerns in developing countries. Occupational exposure to dusts, vapours, and chemical fumes (e.g. mining, construction, manufacturing) are strong COPD risk factors. Genetic Factors Alpha-1 antitrypsin deficiency is a rare but important inherited risk factor. It leads to early-onset emphysema in non-smokers. Asthma and Early-life Respiratory Illnesses Individuals with a history of asthma, recurrent childhood respiratory infections, or low birth weight have a higher likelihood of developing COPD. Age and Gender COPD is more common in people over 40, but emerging data suggests increasing prevalence in women, likely due to rising smoking rates and heightened sensitivity to pollutants. By identifying these COPD risk factors, patients can take preventive steps early. With Cellmaflex, individuals can book routine check-ups, pulmonary screenings, and genetic tests with respiratory specialists without delay. Signs and Symptoms of COPD The early symptoms of COPD can be subtle and are often dismissed as part of ageing or poor fitness. However, recognising these signs can lead to earlier intervention. Key Symptoms Include: Chronic cough (with or without mucus production) Dyspnoea (shortness of breath), initially on exertion, eventually even at rest Wheezing Chest tightness Frequent lower respiratory tract infections Fatigue and exercise intolerance Weight loss in later stages due to increased work of breathing The progressive nature of symptoms underscores the importance of early management. With Cellmaflex, patients can track their symptoms, access imaging and lab reports, and communicate with clinicians remotely for quicker intervention. Diagnosing COPD: Clinical and Functional Approach Accurate diagnosis is vital not only to initiate therapy but also to rule out mimicking conditions like asthma, bronchiectasis, and heart failure. Diagnostic Approach: Medical History & Physical Examination: Focus on smoking history, occupational exposures, and symptom duration. Spirometry: Gold standard. Post-bronchodilator FEV₁/FVC ratio <0.70 confirms airflow limitation. Chest Imaging: X-rays or CT scans reveal hyperinflation, flattened diaphragms, or bullae (especially in emphysema). Arterial Blood Gas (ABG): Assesses oxygen and carbon dioxide levels in advanced disease. Alpha-1 Antitrypsin Testing: Recommended in younger patients (<45 years) or those with no smoking history. Lab Tests: Rule out anaemia, infections, or assess comorbid conditions like heart failure. Cellmaflex makes the entire diagnostic process more seamless, facilitating referrals, viewing results online, and keeping track of spirometry data over time. Living With COPD: Treatment and Long-Term Management While COPD has no cure, treatment focuses on symptom relief, slowing disease progression, and improving quality of life. A. Lifestyle Modifications Smoking cessation: The most effective intervention to slow progression. Cellmaflex can help patients locate cessation programs or nearby pharmacies for nicotine replacement therapy. Avoid triggers: Reducing exposure to dust, fumes, and allergens. Nutritional support: Especially important for underweight patients or those with muscle wasting. Exercise: Pulmonary rehab improves dyspnoea and stamina. B. Pharmacological Therapy Bronchodilators: Short-acting and long-acting
NHS 10 Year Plan in Action: The Role of Cellma in Modernising Healthcare

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents In July 2025, the UK Government unveiled the NHS 10-Year Health Plan for England, titled “Fit for the Future”. The NHS Plan is an ambitious 10-year health plan that lays out plans to tackle the long-standing problems in the NHS by re-imagining care delivery and the functioning of the system, in the face of ever-growing challenges such as demand, workforce problems, and health inequalities. The plan articulates three major shifts. The aim of these shifts is to modernise the services delivered to the population across England and transform their long-term sustainability, accessibility, and equity. It is the aim of NHS England to create healthier lives for everyone, irrespective of where they live or the background of the individual. Over the next decade, the NHS will invest in community-based care; enhance usage of digital tools such as the NHS App, alongside certain initiatives that will help to ensure more GPs will be trained to see the population closer to their home; and halve the gap in healthy life expectancy between the richest and poorest communities. This long-term plan marks a turning point in public health policy, one focused on people, prevention, and progress. What is the NHS 10-Year Plan? The NHS 10-Year Plan sets a detailed roadmap for reform, with milestones extending to 2035. Launched on 3rd July 2025, the plan outlines targeted improvements in care delivery, digital transformation, workforce development, and patient access. The aim is to move from a system strained by hospital admissions and outdated practices to one that is agile, efficient, and digitally connected. One of its major aims is to make sure that 95% of people with complex needs have an agreed care plan by 2027. This claim is made alongside a renewed focus on personalised care and equitable access to personal health budgets (that will be available uniformly by 2035). Financial sustainability is another key objective. The NHS has a backroom requirement to achieve a 2% productivity gain year-on-year for three-years, while changing funding from hospital-based models to community health, and being new models of payment will reward providers for good quality care and outcomes. With a focus on strengthening primary care, using digital capabilities and investing in its workforce, the NHS will be able to meet both day-to-day pressures as well as long-term requirement –making health care not only more efficient but more human. Three Key Shifts in the NHS 10-Year Plan Central to the NHS 10-Year Plan are three strategic shifts designed to modernise and future-proof the delivery of NHS care: From hospital to community: The plan prioritises treating patients closer to home. Community hubs, home visits, and remote consultations will reduce pressure on hospitals and ensure quicker access to NHS services. From analogue to digital: A major technological overhaul is underway. The integration of digital tools will support everything from online appointment booking via the NHS App to AI-assisted diagnostics and fully integrated electronic care records. From treatment to prevention: By investing in early intervention and population health, the NHS aims to reduce avoidable illness. Public health campaigns, targeted screening, and proactive lifestyle management will form a major part of this shift. These changes reflect a broader understanding that healthcare must move beyond traditional models to meet the evolving needs of patients and communities. With more NHS services being delivered locally and supported by smart technologies, the goal is to create a system that is not only responsive, but also predictive and preventative. This evolution will reshape how patients engage with care, moving from one-off interactions to ongoing, tailored support. How Will the NHS 10-Year Plan Improve Patient Care and Access? The NHS 10-Year Plan places patient experience and access at the heart of its transformation. A key priority is to reduce waiting times and make care more convenient by offering same-day appointments, expanding online advice, and investing in out-of-hospital services. These initiatives aim to ensure patients get timely care without unnecessary visits to A&E or long delays. The NHS App is evolving into a central hub for patient engagement. From booking GP appointments to managing prescriptions and accessing medical history, it empowers individuals to take more control of their health. Combined with virtual consultations, these tools allow patients to receive care when and where they need it. Another major development is the emphasis on local care delivery. By shifting services into communities, the NHS is improving outcomes for those with long-term conditions, reducing hospital readmissions, and ensuring follow-up care is more consistent. Importantly, the plan also focuses on reducing inequalities in access. This includes increased funding for underserved regions, expanded outreach services, and the use of data to identify at-risk populations early. In short, the plan ensures that NHS services are not only more efficient, but more inclusive and accessible for all. Key Technological Innovations Supporting NHS Services Technology is a cornerstone of the NHS 10-Year Plan, with bold ambitions to make the NHS the most digitally advanced health system in the world. From AI to genomics, digital innovation will reshape how care is delivered, improving accuracy, efficiency, and patient outcomes. Artificial Intelligence will be embedded across NHS services, helping clinicians make faster, safer decisions. From analysing scans to predicting patient deterioration, AI will play a vital role in early diagnosis and treatment planning. The NHS App is developing into a way to manage appointments, access test results and even get health advice tailored to individual patients in a completely digital experience. Blending digital and in-person services in this way helps patients manage their care from their phones, taking away some of the burden on face-to-face healthcare resources. Further advances in technologies, such as wearables and remote monitoring will help patients track their own health status in real-time, in particular with chronic illnesses, and facilitation of home care for the elderly. Funding for genomic medicine is also being invested by the NHS and with an aim of the everyday use of DNA
Gastroenterology Department Care with Cellma
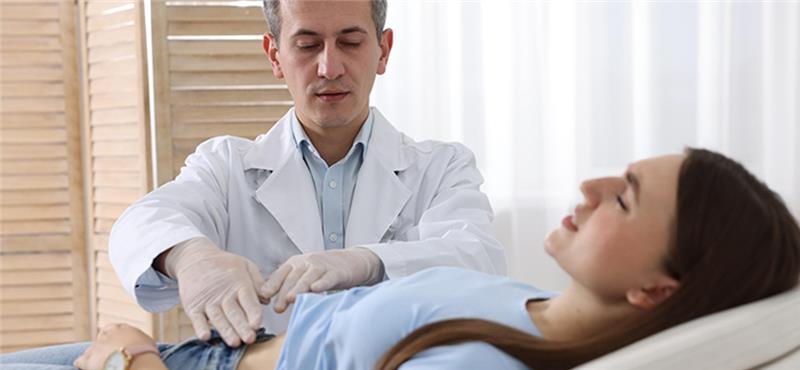
Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents Gastrointestinal diseases impact millions across the world; from the common gastrointestinal infection or chronic inflammatory disease to functional disorders with links to psychological conditions. The gastroenterology department is required to consider the variety of presenting symptoms, perform urgent interventions and develop or initiate an ongoing plan for management across disciplines. Distinction, speed and cross-collaboration are inherently required. Approximately 1 in 5 individuals in the UK experience gastroenteritis each year. About 10–20% of people live with IBS. Disorders of Gut–Brain Interaction (DGBIs) could affect more than 37% of the population. With high demand, digital systems for managing patients need to be a lot more than record keeping. Cellma, an advanced EHR is designed to support the vast complexities involved in a gastroenterology department. Cellma provides clinically intelligent workflows, end-to-end tracking of patients, NHS-ready referral management tools, and real-time integration with diagnostic, imaging, and laboratory systems that help maintain a seamless, structured, and patient-centred plan of care over time, from first consultation to ongoing management. Adhering to NHS Standards and Integrations Cellma is fully compliant with key NHS digital health standards, national and global integrations, ensuring seamless operation in healthcare ecosystem. These include: e-RS (Electronic Referral Service) NHS PDS and CIS2 authentication Summary Care Record (SCR) access SCI Gateway and GP Connect SNOMED CT & ICD-11 coding standards NHS ePrescribing FHIR, HL7 & DICOM interoperability PHS reporting and Data Intelligence ECDS, WECDS, NCCMDS & CSDS datasets Integrated Imaging and Pathology reports This ensures that, within the gastroenterology department, real-time, structured data can be shared across GP practices, laboratories, diagnostic facilities, and hospitals – enhancing clinical accuracy and patient safety. Common Gastroenterological Conditions & Cellma’s Clinical Support In the gastroenterology department, providers manage a broad range of conditions, each with its own diagnostic pathways, multidisciplinary requirements, and associated ongoing care or requirements. Cellma supports the entire clinical pathway and approach that is focused to each diagnosis: Inflammatory Bowel Disease (IBD) Includes Crohn’s disease and Ulcerative colitis, both chronic, relapsing-remitting and immune-mediated diseases. Cellma’s support: Longitudinal tracking of symptoms, flare-ups, calprotectin levels, faecal calprotectin, albumin, CRP, ESR. IBD care plans with clinical dashboards for biologics monitoring, steroid response, and faecal calprotectin timelines. Integration with radiology (CT enterography, MR enterography, MRI pelvis) and endoscopy systems. Multi-team scheduling with IBD nurses, dietitians, surgeons, and hepatologists. Irritable Bowel Syndrome (IBS) and DGBIs Diagnosed via exclusion, and heavily reliant on patient-reported outcomes. Cellma’s support: Symptom diaries with structured questionnaires (e.g., Rome IV Criteria). Digital CBT module integration and dietetic referrals (FODMAP diet support). Data visualisation for long-term symptom triggers and patterns. Liver Disease Includes alcoholic liver disease, Non-alcoholic Fatty Liver Disease (NAFLD), hepatitis, and cirrhosis. Cellma’s support: Integrated Liver Elastography reporting and MELD scoring calculators. Alert-based escalation pathways for transplant referrals. Alcohol liaison and substance misuse service module. Dietetic assessments for hepatic encephalopathy, mental health input for patients with dual diagnosis Gastrointestinal cancers Oesophageal, gastric, colorectal, pancreatic and liver cancers Cellma support: 2-Week-Wait referral triage with automated risk stratification. MDT coordination (oncology, surgery, radiology, pathology) Auto generated follow up and palliative care pathways. Gallbladder and biliary disease Especially in an obese or IBD patient cohort Cellma support: Radiology ordering for ultrasound, MRCP, or HIDA scan. Automated referrals to upper GI surgical teams. Alert to potential complications such as pancreatitis. Key Features of Cellma for Gastroenterology Care Management The gastroenterology department typically deals with patients across seven touchpoints: GP entry, A&E admissions, referrals, triage, specialist assessment, diagnosis and care plan, and long-term follow-up. Cellma solves problems at every level through a clinically deep and unified platform: Clinical Depth and Workflow-Specific Modules: Referral Management: Auto triage-RS referrals by urgency levels (routine, urgent, and 2WW for suspected GI cancer). Diagnostic Integration: Several direct links to imaging, endoscopy, biopsy, histopathology, and laboratory reports on a single screen for a comprehensive review. Structured Assessments: Templates based on Rome IV for IBS assessment, IBD specific scoring (e.g. Mayo, CDAI), and liver scoring (Child-Pugh, Fibrosis). Medication Tracking: Longitudinal drug history for biologics, PPIs, laxatives, corticosteroids, and alerts if there are chances of an adverse event. Multidisciplinary Scheduling: Patient appointment booking across consultants, IBD nurses, dietitians, and mental health clinicians. Virtual Clinics and e-Consents: Pre-built virtual modules for video consultations, remote tracking of symptoms, and e-consents. Solving Real Clinical and Admin Problems: Delayed Diagnosis: By embedding FIT, calprotectin, and full blood panels into the patient timeline Cellma reduces the time to diagnosis. Missed Follow-ups: Alerts are embedded to notify and recall possible missed patients with chronic GI conditions, so they are never lost to follow-up. Depletion of Resources: Cellma platform uses Remote Monitoring tools and Nurse-led Digital clinics to ease the pressure from the consultants and offer the same quality of service. Disjointed Data: Cellma’s single patient view connects all data points—imaging, labs, pathology, medications, letters, and progress notes—into one coherent story. High Admin Load: Auto-generated clinic letters, coded discharge summaries, and real-time task delegation free up hours of clinician time. The gastroenterology department becomes more agile, less paper-reliant, and better able to cope with increasing referrals, complex patient histories, and demand for multidisciplinary input. Data Security and Regulatory Compliance Cellma takes patient confidentiality and data integrity seriously. It meets all national and international security standards: GDPR-Compliant Data Handling Cyber Essentials Plus Certification DSP Toolkit Assessed Role-Based Access Control Fully Encrypted Records and Audit Trails With Cellma, the gastroenterology department can rest assured that patient data is secure, access-controlled, and audit-ready at all times. From acute gastroenteritis to long-term IBD management, the gastroenterology department is expected to deliver accurate, multidisciplinary, and timely care in a highly complex clinical environment. As IBD incidence rises, IBS remains the top outpatient diagnosis, and gut–brain disorders demand psychological input, Cellma is the digital backbone that enables clinicians to deliver care that is clinically rich, safe, and well-coordinated. Whether you’re digitising your referral pathway, managing biologics and diet plans, or running a remote follow-up clinic – Cellma empowers
Asthma Management Starts with Understanding, Continues with Support
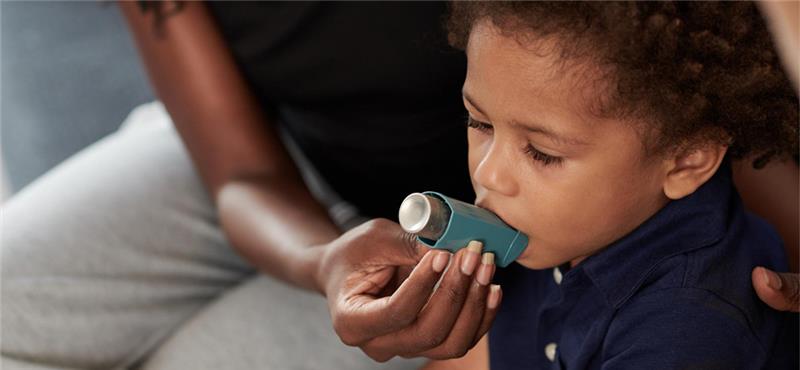
Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents Asthma is not just a cough or wheeze. For millions of people around the world, it’s a daily struggle for enough breath. It shows up uninvited and unwelcome just when you are starting your morning jog, flares up at night when you least expect it or tightens its hold at peak allergy season. No matter if you are a parent trying to soothe your child through a sudden attack, or an adult trying to learn about new symptoms, the impact of having asthma extends far beyond your lungs; it has ramifications in every area of your life. This, however, does not mean that you cannot control your asthma with a good understanding, timely treatment, and ongoing management plan. Cellmaflex makes asthma management easier for patients by allowing them to book their appointments online without calling, look for local doctors through directory, locate pharmacies, labs, or any imaging centre, and most importantly, look at your medical history anytime, anywhere. In this blog, we will take a look at what asthma is, what triggers it, how it is diagnosed and treated, and what living with asthma looks like when supported by a patient-centric solution like Cellmaflex. Why Asthma Awareness Matters Asthma is a lifelong condition that affects the airways in the lungs, making it harder to breathe. For millions worldwide, asthma is not just an inconvenience, it’s a daily challenge that can affect school, work, and physical activities. It can strike at any age, affecting both children and adults, sometimes with little warning. The good news? With the right approach to asthma management, many people live full, active lives. Early diagnosis, trigger awareness, consistent treatment, and access to digital health tools like Cellmaflex can help patients stay ahead of flare-ups. What is Asthma? Asthma is a chronic inflammatory disease of the airways. When exposed to specific triggers, the airway lining becomes inflamed, tighten (bronchoconstriction), and produce excess mucus. This combination narrows the air passages, leading to classic symptoms like wheezing, coughing, and shortness of breath. Flare-ups or “asthma attacks” can vary in intensity. For some, they are mild and occasional; for others, they’re life-threatening and require emergency intervention. According to the Global Asthma Report 2025, it is estimated that over a quarter of a billion people live with asthma worldwide – a number steadily rising due to environmental changes and urbanisation. Additionally, according to the report, asthma affects 9.1% of children, 11% of adolescents and 6.6% of adults, worldwide. This makes asthma management a global health priority. Common Asthma Triggers Understanding your triggers is a cornerstone of effective asthma management. Common triggers include: Allergens: Dust mites, pollen, pet dander, and mould can easily provoke symptoms. Respiratory infections: Even a common cold can aggravate asthma. Air pollution & smoke: Smog, wildfire smoke, or cigarette smoke can worsen inflammation. Weather changes: Sudden temperature drops or dry, cold air often trigger flare-ups. Physical activity: Exercise-induced bronchoconstriction occurs especially during cold-weather workouts. Emotions: Stress or laughter can act as surprising triggers. Food and medication: In rare cases, aspirin, sulphites, or preservatives can induce symptoms. Through Cellmaflex, users can track and record episodes, helping healthcare providers identify and analyse personal triggers faster and more accurately. Signs and Symptoms of Asthma Asthma symptoms can come and go, worsen at night, or flare during specific seasons. Watch out for: Shortness of breath Wheezing (especially when exhaling) Persistent or worsening cough Chest tightness or discomfort Fatigue during or after physical activity Types of Asthma Not all asthma is the same. Here are the main types that influence how asthma management should be approached: Allergic Asthma: Triggered by allergens, often linked with hay fever or eczema. Exercise-Induced Bronchoconstriction (EIB): Occurs during or after physical activity. Occupational Asthma: Caused by exposure to workplace irritants like chemicals or dust. Childhood Asthma: Often begins early and may improve or persist into adulthood. Adult-Onset Asthma: Can start at any age, often more persistent. Severe Asthma: Hard to control even with high-dose medications; needs specialist care. Through Cellmaflex, patients can search for asthma specialists or request a referral for advanced care in their local area. How Asthma is Diagnosed When diagnosing asthma and determining the treatment, a combination of clinical assessment and respiratory tests is used. Medical history: Medical history includes family history, frequency of symptoms, and suspected triggers for asthma symptoms. Spirometry: Measures both how much air a person can exhale and how fast it can be exhaled. Peak Expiratory Flow (PEF): Measures lung performance and is a daily lung performance monitor. Bronchodilator Test: Measures improvement in airflow after using a reliever inhaler. Allergy Testing: Allergy tests may identify and demonstrate triggers that help to explain asthma symptoms. Once asthma is diagnosed, asthma management and treatment should be individualised. Patients who use Cellmaflex also benefit from having all test results and diagnostic records available with the click of a button to quickly obtain second opinions or facilitate shared care. Managing Asthma: What’s Effective There are some common aspects to managing asthma effectively: Controller medications: Most frequently, inhaled corticosteroids are used daily to decrease inflammation. Quick-relief inhalers: Used during asthma flare-ups. Avoidance of triggers: Personalised changes to lifestyle and environment. Asthma action plan: A documented step-by-step plan in consultation with your healthcare provider. Regular check-ups: To assess lung function and monitor the efficacy of treatment. Here is where Cellmaflex comes in by allowing users to digitally store and share their asthma action plans, track their medication or reliever use patterns, and self-book follow-up appointments online. Living with Asthma Asthma does not have to limit your life. With the effective management of asthma, individuals can: Stick to their Asthma management plan: Being adherent is critical. Setting medication reminders on Cellmaflex also helps. Always have quick-relief inhalers available: Always carry your reliever when you are out. Exercise safely: Beneficial warm-ups, breath control and pre-treatment with bronchodilators will help. Create a healthy home: Use air and humidifiers where appropriate. Stay vaccinated: To avoid respiratory infections such as
Improving Community Mental Health Services with Cellma

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents Your browser does not support the audio tag. Community mental health services form the heart of local well-being, ensuring people can access long-term mental health support within their own communities – whether through home visits, outreach programmes, or local health centres. Yet today, these services are under immense pressure. As of April 2024, over 1 million people in the UK were waiting for mental health support. 345,000 referrals had been waiting for over a year, with almost 20% of adults waiting over two years to begin receiving treatment. The delays are just as shocking with children and young people. Almost 110,000 under 18s had waited over 12 months – 49.5% of cases waited over 18 weeks. This is a crisis that community health services can’t solve alone, but with an advanced EHR like Cellma, they can act faster, work better together, and deliver safer, better-coordinated mental health care across every stage of the patient journey. Growing Demand, Limited Capacity: The Strain on Community-Based Care By 2024: 3.6 million had contact with mental health services (increased from 2.6 million in 2016) Over 5 million individuals in one year and regionally across the UK accessed mental health support 640,437 adults and older adults had two or more contacts within the community care 788,000 children and young people had one or more contacts in 2023-24 From rural outreach to youth support groups, community health teams are doing more – but many are hampered by disjointed systems, paper notes, and slow referrals. That’s why Cellma, a leading-edge EHR comes in – not just as a hospital EPR, but as a complete Community EPR that works across disciplines, settings, and services. Conditions Managed in Community Mental Health Services Community teams care for people across a wide spectrum of mental health challenges, including: Schizophrenia and psychosis Bipolar disorder Severe depression and anxiety Obsessive-compulsive disorder (OCD) Post-traumatic stress disorder (PTSD) Borderline and other personality disorders Neurodevelopmental conditions (autism, ADHD) Eating disorders Dual diagnosis (mental illness with substance misuse) Psychosocial challenges linked to housing, employment, trauma, or family breakdown Cellma supports structured care and risk monitoring for each condition with tailored templates and review protocols. Cellma: Designed for Community Mental Health Services Cellma is a comprehensive EHR, built to reflect real-life community care workflows. It enables local providers – community health services, clinics, outreach teams, walk-in centres, social care partners, and voluntary organisations – to manage referrals, assessments, care plans, and crisis support from one secure platform. Whether you’re working in a rural community clinic or an urban outreach programme, Cellma is flexible, multilingual, and locally configurable to your needs. Let’s break down how it supports the complete community mental health care journey: 1. Referral & Triage in Real-Time Referrals come from many sources: GPs, hospitals, schools, local authorities, family services, or even self-referral through integrated care platforms. Cellma enables digital logging and tracking of referrals, classified by level of urgency: Emergency (same day) Urgent (1–5 working days) Routine (within 3 weeks) This triage dashboard provides a real-time view of cases that need priority attention as well as ensuring that referrals are neither missed nor unprocessed. 2. Comprehensive Assessments that are Holistic Cellma is designed to help clinicians and care teams complete comprehensive assessments, either face to face or virtually. Cellma’s tools allow for the completion of assessments including: Mental State Examination (MSE) GAD-7 and PHQ-9 assessments for anxiety and depression HoNOS assessing overall outcomes These assessments can be used to understand an individual’s mental health needs, risk factors and their social setting as part of a larger totality. Once completed, Cellma provides a comprehensive personal Care Plan under the Care Programme Approach (CPA). A personal Care Plan includes; goals, timeframes, crisis situation protocols and care coordinator. 3. Real Multidisciplinary Care in Action Community mental health services are inherently collaborative. Cellma enables multi-disciplinary teams to collaborate within the same digital record. A care team may include, depending on the case: Psychiatrists Community psychiatric nurses Psychologists and therapists Social workers Occupational therapists Peer support specialists Employment or housing advisors Through Cellma; they can write shared notes, develop shared action plans, update medication charts and track goals, while remaining connected and in real time. 4. Monitoring, Reviews & Community Forums Follow-up is critical to long-term mental health recovery. Cellma automatically flags overdue reviews, helps coordinate appointments, and keeps CPA-aligned plans current. 5. Handling Crisis: Responsiveness When It Matters Most Crisis doesn’t wait – and neither should care. Cellma supports emergency responses by connecting patients to: Crisis teams and mobile outreach services Home-based support instead of hospitalisation Mental health liaison teams based in A&E (if applicable) Alerts are triggered for risk factors, missed contacts, or changes in behaviour logged during appointments – so teams can act fast and support individuals in distress. 6. Discharge, Step-Down & Community Reintegration Recovery in mental health is about more than stability – it’s about returning to daily life. Cellma supports transitions: Back to primary care or GP oversight To IAPT or psychological wellbeing services Into voluntary support networks and peer-led groups Discharge planning is fully documented, with handover notes, contact information, and optional post-discharge support like check-in calls or digital follow-ups. Reporting, Integrations & Security – Fully Aligned Cellma helps community care teams deliver high-quality mental health support with: Referral and waiting time reports Risk and incident logs Outcome dashboards using HoNOS, PHQ-9, GAD-7 Caseload management reports Cellma integrates with key systems used in community care: GP Connect NHS Spine & PDS CIS2 EPS (Electronic Prescription Service) for safe, seamless prescribing eRS for referral communication Security and data privacy is comprehensive: End-to-end encryption Role-based access DSP Toolkit Audit logging GDPR-compliant Cyber Essentials Plus certified ISO 27001 accredited At its core, community mental health care is about meeting people where they are. Whether that’s at home, at school, in the clinic, or through outreach – services must be responsive, coordinated, and compassionate. Cellma is built for this reality. From managing soaring
Back Pain & Spine Disorders: A Guide to Better Health

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents The spine is more than just a column of bones; it’s the core structural support system of your body, responsible for supporting movement, maintaining posture, and protecting the spinal cord and nerves. Nonetheless, back issues remain a daily struggle for millions of people, globally. Spinal disorders – specifically lower back pain and sciatica – are frequently reported as some of the most common disabilities in the world. These disorders can hinder mobility, productivity, and quality of life. According to WHO, in 2020, low back pain (LBP) impacted 619 million people globally, and it is predicted the number of cases will rise to 843 million cases by 2050, largely due to population growth and ageing. In this situation, our digital health platform - Cellmaflex, provides everything you need to understand and manage your spinal health more effectively. This includes online appointment booking, no need for phone calls, access to your medical history, and the ability to locate nearby doctors, pharmacies, labs, and imaging centres. All your medical needs in one platform. In this blog, we will explore: the most common symptoms of spine disorders, structural and neurological causes, postural and mechanical back complaints, systemic and inflammatory spinal conditions, injury-related and lifestyle factors, and management to improve outcomes. Most Common Signs & Symptoms of Spine & Back Disorders Spinal disorders may progress slowly or suddenly, often beginning with mild symptoms and progressing to chronic or debilitating pain. Warning signs include: Persistent or recurring lower back pain Pain that radiates down one or both legs (especially in sciatica) Tingling, numbness, or weakness in the lower limbs Limited mobility or stiffness in the lower back Pain that worsens with sitting, standing, or lifting Recognising these symptoms early can make a significant difference. Structural and Nerve-Related Disorders These spine disorders involve physical changes in the spinal structure or direct nerve compression: Herniated Disc: A spinal disc may bulge or rupture, pressing on nearby nerves and causing pain, numbness, or weakness. It’s most common in the lumbar (lower back) region. Sciatica: Caused by irritation or compression of the sciatic nerve (the largest nerve in humans, originating in the lower back and traveling posteriorly through the lower limb as far down as the heel of the foot). Sciatica leads to sharp, shooting pain down the leg, often on one side. It may also cause burning, numbness or tingling sensations. Spinal Stenosis: This is a narrowing of the spinal canal, often due to arthritis or disc degeneration, which puts pressure on the spinal cord or nerves. Symptoms include pain, weakness, or difficulty walking. Cellmaflex helps patients manage these conditions by offering quick access to their radiology reports, enabling better-informed discussions with orthopaedic or neurological specialists. Postural and Mechanical Back Problems Not every spine disorder is due to major structural issues, many stem from habits and mechanical stress: Lower Back Strain: Bending or overstretching of a muscle or ligament is often due to lifting something heavy incorrectly, sudden movements, or twisting. It can also be simple overuse. Degenerative Disc Disease: As the years go by, the spinal discs lose water content and elastin, which reduces the ability of the disc to absorb pressure and to cushion the vertebrae. This means chronic back pain and stiffness. Scoliosis: This refers to anything ranging from normal postural action to an abnormal curvature of the spine. Usually, this is associated with lateral curvature, attendant, uneven shoulders or hips and chronic discomfort. Spinal problems of this type often respond well to physical therapy and posture retraining. Cellmaflex allows you to schedule rehab sessions and record improvements in your back health over time. Systemic & Inflammatory Conditions Affecting the Spine Some spine disorders, while less common, are systemic and sometimes inflammatory, including: Arthritis of the Spine: Generally seen in adults as a feature of aging; this inflammation of the joints of the spine can lead to pain and stiffness. Sometimes, this pain is especially noticeable after resting. Ankylosing Spondylitis: A chronic inflammatory condition that primarily affects the spine and sacroiliac joints. It causes pain and stiffness that typically worsens with rest and improves with activity. Over time, it can lead to the fusion of spinal vertebrae, limiting mobility. These conditions require ongoing care and monitoring. Cellmaflex makes it easier to coordinate with rheumatologists and track lab tests, imaging, and medication effectiveness, all in one place. Injury-Related and Lifestyle-Linked Disorders: Some spine disorders result from trauma, overuse, or modern lifestyle factors: Sprains, Fractures, or Disc Injuries: Back injuries from falls, car accidents, or sports can result in acute pain and long-term complications if not properly treated. Poor Ergonomics or Sedentary Lifestyle: Sitting for long hours, poor posture, and lack of exercise lead to muscle imbalances, stiffness, and back pain. Tips for Prevention & Care: Use proper lifting techniques Maintain a healthy weight Exercise regularly to strengthen back muscles Invest in ergonomic furniture for workstations Cellmaflex can help you locate physiotherapists, track your rehabilitation plan, and access self-care tips to support daily back health. Intervention & Management Managing a spine disorder requires a holistic and individualised approach: Medications: Pain relievers, muscle relaxants, or anti-inflammatories may be prescribed to manage symptoms. Physical Therapy: Targeted exercises improve flexibility, core muscle strength, and promote proper posture. Lifestyle Modifications: Movement (exercise), a balanced diet, hydration, and a healthy BMI can effectively reduce strain on the back. Ergonomics: Use supportive chairs, lumbar pillows, standing desks, and proper lift techniques to avoid repeat back pain. While back pain is common, it should never be ignored, especially when it becomes persistent or radiates to the legs. Spine disorders can significantly impair your quality of life, but with an early diagnosis, targeted intervention, and lifestyle changes, many cases can be navigated or even prevented. Don’t wait until the pain becomes severe. Consult a healthcare provider if you’re experiencing symptoms. Use Cellmaflex to simplify your health care journey by finding doctors, managing your records and tracking your progress.
Health Visitors Empowered by Cellma for Safer Care

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents Health visitors are the public health professionals whose primary role is to support children and families during the critical early years in a child’s life. They are the health professionals who are in families’ homes and communities, helping them to be as healthy and safe as possible in all aspects of health: physical, emotional, and developmental. When public health needs are increasing and safeguarding processes are more complex, digital support through an advanced EHR – Cellma enables health visitors to provide safe, effective, timely, and holistic care to families. This blog showcases how Cellma, as a fully integrated electronic patient record (EPR) system, supports all areas of practice for a health visitor from safeguarding to developmental checks, referrals and reporting. Cellma helps health visitors to achieve the requirements established by NICE and NHS Why Health Visiting Matters More Than Ever Recent national data paints a concerning picture. In 2023–24: 399,460 children were classed as in need. 224,520 child protection enquiries were initiated. 49,990 children were on child protection plans. 18.2% of infants missed their 6–8-week review on time. Over 21% of children were not seen for their 2–2½-year review. While referrals have reduced the number of child protection enquiries remain at a high level, especially for neglect. In this scenario health visitors have a unique preventative role and require tools that enable them to focus on population health as well as individual care journeys. Health Visitors’ Role in Safeguarding and Early Intervention Health visitors are in a remarkable position to be the first service responding to early warning signs, which might range from domestic violence or drug misuse to developmental deficits, and should be able to comply with the Needs Assessment and support vulnerable families with protective strategies in a timely response. Key responsibilities of health visitors include: Attending Child in Need (CIN) and Child Protection (CP) case conferences. Supporting Looked After Children (LAC) with routine and statutory health assessments. Conducting home visits and health needs assessments. Sharing concerns and updates with social workers, GPs, schools, and police. Leading Early Help assessments to pre-empt crisis situations. How Cellma helps: Health visitors can record, access, and share safeguarding notes securely with authorised professionals. Automated reminders ensure no visit or review is missed. Multi-agency updates are synchronised in real time, enhancing visibility and actionability. Safeguarding Built In – Because Safety Starts with Awareness In health visiting, safeguarding is not a function – it’s a duty. Cellma is designed for clinicians to allow for the detection, documentation, and escalation of safeguarding concerns through workflows and alerts to aid proactive child protection. CP-IS Integration Cellma integrates with Child Protection – Information Sharing (CP-IS), providing authorised users with instant access to a child’s protection status and social care plan. This is essential in emergency and unscheduled care environments such as A&E, maternity, paediatric wards, GP out-of-hours, 111 service, ambulance teams, SARCs and others. Safeguarding flags will show up in the patient’s summary, making the clinical decision support information available quickly for informed decisions. Safeguarding Alerts Based on narrative clinical notes, coded data or combinations of symptoms – Cellma alerts staff that immediate action is required and justify concerns with possible harm. Structured Safeguarding Pathways Fully customisable templates for child protection plans, LAC documents, MASH, CAMHS, Early Help, and multi-agency referrals – all with timelines, actions. Embedded Care Plans Shared care plans for safeguarding situations, with named worker responsibilities, contact histories, alerts for parental mental health or substance misuse, domestic abuse and social care involvement – all version-controlled and audit-ready. Audit-Quality Documentation Every action taken is time-stamped, traceable, and aligned to CQC and statutory reporting requirements, giving paediatric teams assurance of no red flag being unobserved. From initial check-in to follow-up case management, Cellma makes safeguarding visible, structured, and central to child healthcare delivery. Child Developmental Checks Made Smarter with Cellma Health visitors routinely monitor a child’s growth, physical and emotional development, and family dynamics. Key health checks include: New birth visit (10–14 days) 6–8-week check 12-month review 2–2½-year developmental check (including ASQ-3 screening) Cellma’s health visiting module supports: Automated scheduling and alerts for due and overdue checks. Input of growth metrics like weight, head circumference, and height. Capture of ASQ-3 scores and red flags for early intervention. Maternal mental health questionnaires with flagging for perinatal mental health referrals. Referral Pathways: A Seamless Process with Cellma Health visitors are responsible for identifying needs and ensuring families are connected with the right services. These may include: Speech and Language Therapy (SALT) CAMHS or neurodevelopmental teams (for suspected autism or ADHD) Community Paediatrics Dietetics and nutrition advice Housing support teams Family hubs, parenting support, and community groups With Cellma, these referrals are: Logged within a central EPR. Linked to outcomes tracking. Auto routed to the correct departments with updates visible to the original referrer. Accompanied by relevant clinical notes and developmental concerns. Clinical Conditions Managed by Health Visitors Beyond the social and developmental responsibilities, health visitors are trained to manage or identify a range of clinical conditions Feeding difficulties and faltering growth Childhood eczema, allergies, and skin issues Constipation and toileting issues Immunisation education and catch-up planning Maternal postnatal depression and anxiety Sleep and behavioural concerns Oral health education and dental referrals Unexplained injuries or bruises (often first noticed during home visits) Cellma allows structured templates for clinical documentation, early warning scores, symptom tracking, and integration with GP and paediatric systems reducing duplication and enabling proactive care. BI Reporting, NICE Compliance, and Timely Documentation Health visiting is governed by multiple standards and reporting frameworks, from the Healthy Child Programme to NHS Digital data returns. Cellma’s advanced BI reporting tools and compliance features ensure: Reports on missed or late visits and reviews. Audit trails of safeguarding activity and multi-agency engagement. Real-time dashboards to flag regional or demographic risks. Data extraction for public health reporting, inspections, and funding reviews. Alignment with NICE guidelines and local authority frameworks. Supporting Diverse and Changing Populations with Cellma The demographic landscape is evolving: Children in need are increasingly older
Muscle Disorder: Signs, Causes & How to Take Control

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents Your muscles do not only facilitate movement: they help to maintain balance; they assist with breathing; and they help us to complete daily tasks. However, what happens if something happens to your muscle’s health? The consequences that arise from a muscle disorder can greatly impact how you move, how you live, and how you feel; they can even affect your autonomy and the quality of your day-to-day living. With digital tools like Cellmaflex, managing muscle health can be made easy. With Cellmaflex you can book appointments online without having to make phone calls, access your medical history anytime, anywhere, or search for the nearest doctors, pharmacies, labs and imaging centres, all in one place. In this blog, we will address what defines a muscle disorder, outline the significance of looking after muscle health, discuss the different types and aetiology of muscle disorders, including describing the major signs and symptoms to watch for, and showing you how Cellmaflex can assist your journey to care. What Is a Muscle Disorder? A muscle disorder is any problem that affects muscle tissue’s structure or function. It may affect strength, endurance, coordination, or ability to do everyday tasks. Depending on the cause and when it is treated, a muscle disorder may be temporary or permanent, mild or severe disability. From genetic conditions like muscular dystrophy to lifestyle-related injuries like tendonitis, muscle disorders take many forms but they all require timely diagnosis and consistent care, which Cellmaflex helps support by enabling seamless access to health records and specialist referrals. Muscle-related conditions are growing in global prevalence. According to the World Health Organisation (WHO) and Global Burden of Disease 2025 Report, musculoskeletal disorders affect over 1.7 billion people worldwide and are the leading cause of global disability. Muscle disorders (including genetic, inflammatory, and metabolic types) are projected to affect over 300 million people in 2025. The Importance of Muscle Health Muscles are central to mobility, posture, metabolism, and even internal organ function. When muscles are weakened, inflamed, or degenerated, the entire body suffers. From a child struggling to play to an adult unable to work or care for themselves, muscle disorders impact quality of life, independence, and mental health. This is why early diagnosis, rehabilitation, and a multidisciplinary care approach, easily managed through a unified platform like Cellmaflex, are vital to long-term outcomes. Common Signs & Symptoms That Indicate a Muscle Disorder Many disorders start subtly. Look out for: Persistent muscle weakness (e.g., trouble lifting objects, climbing stairs) Muscle pain or cramps that don’t improve with rest Fatigue, especially during or after simple activities Muscle twitching or spasms Decreased range of motion or flexibility Trouble with balance or coordination If you experience any of these signs, you can use Cellmaflex to book a consultation with a neurologist or rheumatologist. Genetic and Neuromuscular Disorders These disorders are either inherited, or spontaneous changes in particular genes or develop due to problems in the nervous system’s communication with muscles. Muscular Dystrophy A group of genetic disorders that causes progressive muscle wasting. Symptoms usually begin in childhood and worsen over time. Common types include Duchenne and Becker muscular dystrophies. Amyotrophic Lateral Sclerosis (ALS) Also known as Lou Gehrig’s disease, ALS affects motor neurons, leading to muscle paralysis. It progresses rapidly, impacting breathing and swallowing. Myasthenia Gravis An autoimmune neuromuscular disorder where antibodies block communication between nerves and muscles. It causes muscle fatigue, drooping eyelids, and trouble speaking or swallowing. Inflammatory and Autoimmune Muscle Myopathies These involve the immune system attacking healthy muscle tissues. Myopathy Inflammatory myopathies like polymyositis and dermatomyositis lead to chronic inflammation, weakness, and skin rashes. Symptoms can be slow to appear and often overlap with other conditions, making consistent monitoring essential. Other autoimmune muscle disorders include: Inclusion body myositis: Gradual onset weakness in hands and thighs Polymyositis: Symmetrical muscle weakness, often seen in adults Metabolic and Systemic Muscle Conditions When the body’s metabolism or systems, like the endocrine or renal systems, are disrupted, muscle function can be affected. Injury-Related and Overuse Disorders These are often caused by physical strain, repetitive motion, or improper posture. Tendonitis Inflammation of tendons (connecting muscle to bone) due to overuse. Common types include: Rotator cuff tendonitis (shoulder) Tennis elbow (elbow) Patellar tendonitis (knee) These injuries are common in athletes, manual workers, and those with repetitive daily tasks. Detecting and Treating Muscle Disorders Muscle disorders can start slowly but have long-lasting repercussions if not treated. They can affect people in every life stage involving genetic, inflammatory, metabolic or injury related causes. The key to avoiding complications and preserving quality of life is identification in the initial stages when changes first occur. Important Steps to Manage Muscle Disorders Diagnosis: A complete health assessment is the first step to diagnosing the muscle disorder! Think about: A physical examination and neurological assessment Blood tests to look for muscle enzymes, inflammation or autoimmune indicators Electromyography (EMG) or nerve conduction studies Muscle biopsies or genetic tests (for inherited disorders) Treatment Approaches: Treatment depends on the type of muscle disorder, but usually includes: Medications: anti-inflammatories, immunosuppressants or enzyme replacement Physical therapy: to improve strength, flexibility and minimise contractures Occupational therapy: to help learn to adapt daily activities to maintain independence Nutritional support: mainly in metabolic muscle disorders Surgery: in rare cases, to rectify deformities or relieve nerve compression Long-Term Care: Chronic muscle disorders need to be monitored over time and have multi-disciplinary support, and may include: Regular reviews with neurologist, rheumatologist or physiatrist Adapting plans as disease state changes Introducing changes in lifestyle – gentle exercise, balanced diet and stress management Importance of Taking Action so that You Can Improve Your Mobility and Quality of Life Taking the first step, by first identifying muscle disorders through your own awareness and active treatment strategy, will help limit permanent damage, increase mobility and improve quality of life. The first step is knowledge, body awareness, and medical care when needed to protect the health of
Cellma Powers Efficient, Compliant District Nursing Care

Table of Contents Help Others Discover – Click to Share! Facebook Twitter LinkedIn Table of Contents District nursing plays a pivotal role in bridging the gap between hospital and homecare; clearly supporting patients with complex, ongoing, and often palliative needs whilst enabling them to navigate the complexities of their life in the community. The increase in demand persists, whilst NHS trusts are not only experiencing a decreased workforce, but also an increased number of referrals and the need for accessible, interoperable and efficient care. This is where Cellma comes in; an advanced EHR software that not only supports district nursing teams but has the capacity for district nursing teams to deliver timely, coordinated and compliant care more uniformly across geographical boundaries. In this blog, we will explore the full spectrum of district nursing workflows, how Cellma supports each stage of care, and how it aligns with national standards, governance frameworks, and the evolving needs of patients and providers alike. District Nursing: The Clinical Backbone of Community Care Often overlooked yet fundamentally essential, district nursing provides clinical care to patients in their own homes, care homes, and community settings. Services are typically targeted at older adults as well as children with complex or multiple chronic conditions and wound management, recent hospital discharges, or palliative care needs. Recent statistics show that in 2021 alone, district nursing teams carried out 307,783 patient contacts across just under 20,000 individuals – averaging nearly 16 home visits per patient. Nearly half of these patients were aged 70 and above, and the majority were women. Yet, despite this growing demand, the number of district nurses in England dropped by 43% between 2009 and 2019. This leaves just one district nurse per 14,000 people – a sharp contrast to the GP-to-patient ratio of 1:1,600. With such intense pressures, a robust digital foundation is no longer optional. It’s essential. That’s where Cellma offers unmatched value. Conditions Managed in District Nursing District nursing covers a broad spectrum of medical conditions, including: Wound care (e.g., pressure ulcers, venous leg ulcers) Diabetes management COPD and asthma Cancer and palliative care Dementia support Stroke and orthopaedic rehabilitation Cellma ensures that all condition-specific care plans are backed by clinical templates, alerts, and decision-support logic. This helps standardise care while preserving the flexibility for personalised approaches. Streamlined Referrals and Caseload Management District nursing teams receive hundreds of new referrals daily. In some NHS Trusts, that number reaches 200 new referrals per day. These come from GPs, hospital discharge coordinators, social care services, and sometimes carers or the patients themselves. The Referral Portal in Cellma allows swift intake and digital triage. Each referral is triaged by urgency and complexity using flexible triage tools. The system allows for automated case routing which ensures that nurses and regions have equitable caseloads. Managers can see the caseloads in real-time, allowing them to make reactive staffing decisions and avoid bottlenecks. Evidence has shown that using Cellma, some Trusts have achieved wait times of below five days and prevented missed visits altogether. Digital Assessments with Wound Charting, Combined with Visual Tools Initial assessments are critical to establish care pathways and goals. Cellma allows for mobile-ready digital forms that support: Capturing full patient history such as medical, surgical and medication Physical assessments including mobility, nutrition, pressure ulcer risk (e.g: Waterlow)and pain level Mental health and cognitive screenings such as GAD-7, PHQ-9. Environment and safeguarding checklists Risk matrix scoring, and documentation aligned with child and adult protection frameworks A standout feature is Cellma’s interactive wound charting tool. This tool allows nurses to visually document wound sites, sizes, and healing progression over time. Nurses can also upload photos securely, annotate diagrams, and apply standardised wound scoring tools (e.g., PUSH Tool, TIME framework). These visual inputs are crucial for team collaboration, escalation, and continuity. Clinical Interventions and Personalised Care Pathways District nurses deliver a wide range of hands-on clinical interventions such as: Wound management Catheter and continence care with bladder/bowel assessments, catheter passport tracking, and fluid balance monitoring. Medication administration Post-operative care Palliative and end-of-life support With Cellma’s care pathway, nurses follow condition-specific protocols embedded directly in Cellma. When managing chronic wounds, diabetic problems, or follow-up monitoring of discharge arrangements for people discharged from cardiac inpatient services, Cellma helps to ensure that the care planned is based on evidence-based systems. Pathways can be tailored for each individual patient and can automatically generate tasks, alerts, and review timelines. Communication with GPs and Multidisciplinary Teams Cellma’s Communication Module is designed specifically for integrated care delivery. Cellma supports UCR (urgent community response) compliance with response time tracking, prioritised triage, and rapid access care pathways aligned with the 2-hour standard. District nurses can: Create structured letters to GPs (both contingency plans or requests for medication changes, dosages, or requests for specialist review) Cellma enables structured data sharing with GP systems via FHIR-compatible messaging or GP Connect record views. Request responses from authorities, social or allied health services and record them Request and host MDT meetings and share working notes such as care plans and clinical notes. There are reduced delays in decision-making and the best-case prescribing safety and supply, particularly important when urgent interventions (i.e., urgent change of an anticoagulant dose or new pain management plan) are going to be initiated in the community setting. Monitoring, Reviews, and Real-Time Documentation Ongoing Reviews are important in District Nursing, because many of the patients we care for have an up and down journey with varying health conditions. Cellma provides: Daily or weekly monitoring log Automated alerts to notify teams of declining symptoms Team dashboards for joint tracking Profile notes and voice capture to reduce admin Real-time visibility allows teams to adjust the frequency of visits, escalate concerns and hold additional MDT discussions. Safe Discharge and Follow-Up Coordination Patients exit district nursing services when they have recovered, stabilised, or transitioned to long-term care. With Cellma, discharges are handled using structured workflows. Discharge letters, medication reconciliations, and handover documents can be digitally generated and automatically shared with the relevant GP or social care provider.


